FETAL MALPRESENTATIONS. PREGNANCY AND DELIVERY AT BREECH PRESENTATION. DEFLEXIO CAPITIS.
Prepared by I. Kuziv
Usually the fetal head engages in the occipito-anterior position (more often left occipito-anterior (LOA) rather than right) and then undergoes a short rotation to be directly occipito-anterior in the mid-cavity. Malpositions are abnormal positions of the vertex of the fetal head relative to the maternal pelvis. Malpresentations are all presentations of the fetus other than vertex.
MALPRESENTATION
Predisposing factors to malpresentation include:
· Prematurity.
· Abnormalities of the uterus, eg fibroids.
· Partial septate uterus.
· Abnormal fetus.
Breech pregnancy: Introduction
Breech pregnancy is a condition of pregnancyin which the fetus or baby is not in the head-down position in the uterus. Breech pregnancy is common and normal in early pregnancy as the baby grows and moves around in the uterus. However, by about 36 weeks of pregnancy, the baby should have moved into the head-down position, the normal position for vaginal delivery. If this has not happened, it is called a breech presentation.
In a breech pregnancy or breech presentation, the baby is positioned with the buttocks down and the head up. The mother may or may not be aware of any symptoms of a breech pregnancy or breech presentation. Complications of breech pregnancy that lead to breech presentation and a vaginal breech delivery can include difficult vaginal delivery, fetal distress, birth defects and compression of the umbilical cord. For more details on symptoms and complications, refer to symptoms of breech pregnancy.
One of the main causes of a breech pregnancy that leads to a breech presentation is prematurity. Risk factors for breech pregnancy that leads to a breech presentation include having an abnormally shaped uterus, too little or too much amniotic fluid, having twins, triplets or other multiple pregnancies, fibroids of the uterus and placenta previa.
There are several variations of a breech pregnancy orbreech presentation. These include a frank breech presentation, in which the hips of the fetus are flexed and the legs extend straight upward with the knees straight and the feet at the head or face.
A breech pregnancy or breech presentation called a complete breech presentation occurs when the hips and the knees of the fetus are flexed. A breech pregnancy or breech presentation called a footling breech presentation occurs when one or both of the infant's feet cover or push through the cervix of the uterus.
A breech pregnancy that results in a breech presentation occurs in only about 3 percent to 5 percent of pregnancies with a single infant. A breech pregnancy that results in a breech presentation is more common in multiple pregnancies, in which there are twins, triplets or other multiple infants.
A diagnosis of breech pregnancy and/or breech presentation is made by ultrasound. In the later stages of pregnancy, it is often possible for a licensed physician or nurse midwife to feel a breech presentation through the wall of a pregnant woman's abdomen. A variety of other tests may be performed to evaluate overall health of the mother and the fetus. Tests can include blood tests, such as a complete blood count (CBC), a chemistry panel, urinanalysis, and blood glucose testing. Amniocentesis may also be performed for some women.
It is possible that a diagnosis of breech pregnancy can be missed or delayed. For more information on misdiagnosis, refer to misdiagnosis of breech pregnancy.
Breech pregnancy can be treated or addressed to minimize any complications that can occur during labor and delivery. Treatment can include manual manipulation to turn the baby into the correct head-down position (vertex presentation). This is called external cephalic version.
Infants in a breech presentation that are unable to be repositioned into the vertex position are often delivered by cesarean section. In some cases it is possible to safely deliver an infant vaginally in abreech presentation. For more information on treatment, refer to treatment of breech pregnancy.
Breech pregnancy: Symptoms
Many women are unaware of a breech pregnancy, especially in early pregnancywhen the baby is small and tends to move around and shift positions often. If the infant remains in a breech presentation and does not move into a head-down position (vertex presentation) in late pregnancy, a woman may be able to feel the baby's head in the upper area of the abdomen and/or possibly a lot of kicking or movement in the lower abdomen.
A breech pregnancy can often be felt through the abdomen by a licensed physician of nurse midwife in late pregnancy. Other clinical signs of a breech pregnancy can be seen on an imaging test called an ultrasound. These include a position in which the infant's buttocks are down and seated against the cervix of the uterus and the head is at the top area of the uterus.
Breech presentation
· Breech presentation is the most common malpresentation, with the majority discovered before labour. Breech presentation is much more common inpremature labour.
· Approximately one third are diagnosed during labour when the fetus can be directly palpated through the cervix.
· After 37 weeks, external cephalic version can be attempted whereby an attempt is made to turn the baby manually by manipulating the pregnant mother's abdomen.
· If the pelvis is normal and estimated fetal weight is 2,500-4,000 g, assisted breech delivery with experienced staff is believed to be as safe asCaesarean section;[1] approximately 50% of women aiming for vaginal delivery will achieve this.
· Women who have an elective Caesarean section for a breech presentation in their first pregnancy have approximately a 1 in 10 chance of having an elective Caesarean section for a breech presentation in their second pregnancy.[2]
Transverse lie
· When the fetus is positioned with the head on one side of the pelvis and the buttocks in the other (transverse lie), vaginal delivery is impossible.
· This requires Caesarean section unless it converts or is converted late in pregnancy. The surgeon may be able to rotate the fetus through the wall of the uterus once the abdominal wall has been opened. Otherwise, a transverse uterine incision is needed to gain access to a fetal pole.
· Internal podalic version is no longer attempted.
Malposition
Occipito-posterior position
· This is the most common malposition where the head initially engages normally but then the occiput rotates posteriorly rather than anteriorly. Approximately 10% of labours begin this way, but many correct in labour.
· The occipito-posterior position results from a poorly flexed vertex. The anterior fontanelle (four radiating sutures) is felt anteriorly. The posterior fontanelle (three radiating sutures) may also be palpable posteriorly.
· It may occur because of a flat sacrum, poorly flexed head or weak uterine contractions which may not push the head down into the pelvis with sufficient strength to produce correct rotation.
· Occasionally, epidural analgesia relaxes the pelvic floor such that the occiput sinks into it instead of being pushed to the correct position.[3]
Management
· As occipito-posterior position pregnancies often result in a long labour, close maternal and fetal monitoring are required. An epidural is often recommended and it is essential that adequate fluids be given to the mother.
· The mother may get the urge to push before full dilatation but this must be discouraged. If the head comes into a face to pubis position then vaginal delivery is possible as long as there is a reasonable pelvic size. Otherwise, forceps or Caesarean section may be required.
Occipito-transverse position
· The head initially engages correctly but fails to rotate and remains in a transverse position.
· Alternatives for delivery include:
· If the second stage is reached, the head must be manually rotated with Kielland's forceps or delivered using vacuum extraction. This is inappropriate if there is any fetal acidosis because of the risk of cerebral haemorrhage.
· Therefore, there must be immediate provision for a failure of forceps delivery to be changed immediately to a Caesarean. The trial of forceps is therefore often performed in theatre.
· Some centres prefer to manage by Caesarean section without trial of forceps.
Face presentations
· Face presents for delivery if there is complete extension of the fetal head.
· Face presentation occurs in 1 in 300 deliveries.
· With adequate pelvic size, and rotation of the head to the mento-anterior position, vaginal delivery should be achieved after a long labour.
· Backwards rotation of the head to a mento-posterior position requires a Caesarean section.
Brow positions
· The fetal head stays between full extension and full flexion so that the biggest diameter (the mento-vertex) presents.
· Brow presentation occurs in 1 in 500 deliveries.
· Brow presentation is usually only diagnosed once labour is well established.
· The anterior fontanelle and super orbital ridges are palpable on vaginal examination.
· Unless the head flexes, a vaginal delivery is not possible, and a Caesarean section is required.
What causes breech position during pregnancy?
There is often no clear reason why the baby did not turn head-down. In other cases, breech position might be linked to:2
· Labor that begins before the 37th week of pregnancy, before the baby is likely to turn head-down on its own.
· Twins or more. Limited space for two or more babies can prevent them from moving into the head-down position before delivery.
· Too much or too little amniotic fluid in the uterus.
· Problems with the uterus, such as an oddly shaped uterus or uterine fibroids, which are noncancerous growths in the uterine wall.
· Stretched and weakened uterine muscle from past pregnancies.
· Problems with the baby, including heart, digestive tract, and brain problems, such as Down syndrome, anencephaly, or hydrocephalus.
BREECH PRESENTATION
Breech presentation is common remote from term. Most often, however, some time before the onset of labor the fetus turns spontaneously to a cephalic presentation so that breech presentation persists in only about 3 to 4 percent of singleton deliveries. For example, 3 percent of 58,334 singleton infants delivered from 1991 through 1994 at Parkland Hospital presented as breech.

As term approaches, the uterine cavity most often accommodates the fetus in a longitudinal lie with the vertex presenting. Factors other than gestational age that appear to predispose to breech presentation include uterine relaxation associated with great parity, multiple fetuses, hydramnios, oligohydramnios, hydrocephalus, anencephalus, previous breech delivery, uterine anomalies, and pelvic tumors.

There are three types of breech presentation: complete, incomplete, and frank.
Complete breech is when both of the baby's knees are bent and his feet and bottom are closest to the birth canal.
Incomplete breech is when one of the baby's knees is bent and his foot and bottom are closest to the birth canal.
Frank breech is when the baby's legs are folded flat up against his head and his bottom is closest to the birth canal.
There is also footling breech where one or both feet are presenting.
Fianu and Vaclavinkova (1978) provided sonographic evidence of a much higher prevalence of placental implantation in the cornual–fundal region for breech presentations (73 percent) than for vertex presentations (5 percent). The frequency of breech presentation is also increased with placenta previa, but only a small minority of breech presentations are associated with a previa. No strong correlation has been shown between breech presentation and a contracted pelvis.
A live fetus is not required for a fetus to change presentations spontaneously. One woman admitted to Parkland Hospital at term had a fetus known to be dead, confirmed by real-time sonography. The presentation was cephalic during the first oxytocin induction. Three days later, at the time of the second attempt at labor induction, the fetus was in a breech presentation. Three days later, at the time of a third and successful induction, the fetus was again in a cephalic presentation!
In the persistent breech presentation, an increased frequency of the following complications can be anticipated:
(1) perinatal morbidity and mortality from difficult delivery;
(2) low birthweight from preterm delivery, growth restriction, or both;
(3) prolapsed cord;
(4) placenta previa;
(5) fetal, neonatal, and infant anomalies;
(6) uterine anomalies and tumors;
(7) multiple fetuses;
and (8) operative intervention, especially cesarean delivery.
The varying relations between the lower extremities and buttocks of breech presentations form the categories of frank, complete, and incomplete breech presentations. With a frank breech presentation, the lower extremities are flexed at the hips and extended at the knees, and thus the feet lie in close proximity to the head. A complete breech presentation differs in that one or both knees are flexed. With incomplete breech presentation, one or both hips are not flexed and one or both feet or knees lie below the breech, that is, a foot or knee is lowermost in the birth canal. The frank breech appears most commonly when the diagnosis is established radiologically near term.

Fig. 1 Longitudinal lie. Frank breech presentation.

Fig. 2 Longitudinal lie. Complete breech presentation.

Fig. 3 Longitudinal lie. Incomplete, or footing, breech presentation.
Classification
of breech presentations
ABDOMINAL EXAMINATION
Typically, with the first Leopold maneuver, the hard, round, readily ballottable fetal head is found to occupy the fundus (Fig. 4). The second maneuver indicates the back to be on one side of the abdomen and the small parts on the other. On the third maneuver, if engagement has not occurred—that is, if the intertrochanteric diameter of the fetal pelvis has not passed through the pelvic inlet—the breech is movable above the pelvic inlet. After engagement, the fourth maneuver shows the firm breech to be beneath the symphysis. Fetal heart sounds are usually heard loudest slightly above the umbilicus, whereas with engagement of the fetal head the heart sounds are loudest below the umbilicus.

Fig. 4 Palpation in left sacroanterior position. A. First maneuver. B. Second maneuver. C. Third maneuver. D. Fourth maneuver.
VAGINAL EXAMINATION
With the frank breech presentation, both ischial tuberosities, the sacrum, and the anus are usually palpable, and after further descent, the external genitalia may be distinguished. Especially when labor is prolonged, the buttocks may become markedly swollen, rendering differentiation of face and breech very difficult; the anus may be mistaken for the mouth, and the ischial tuberosities for the malar eminences. Careful examination, however, should prevent this error, because the finger encounters muscular resistance with the anus, whereas the firmer, less yielding jaws are felt through the mouth. Furthermore, the finger, upon removal from the anus, is sometimes stained with meconium. The mouth and malar eminences form a triangular shape, while the ischial tuberosities and anus are in a straight line. The most accurate information, however, is based on the location of the sacrum and its spinous processes, which establishes the diagnosis of position and variety.
In complete breech presentations, the feet may be felt alongside the buttocks, and in footling presentations, one or both feet are inferior to the buttocks (Fig. 18). In footling presentations, the foot can readily be identified as right or left on the basis of the relation to the great toe. When the breech has descended farther into the pelvic cavity, the genitalia may be felt.

Fig. 5. Double-footling breech presentation in labor with membranes intact. Note possibility of umbilical cord accident at any instant, especially after rupture of membranes.
X-RAY, COMPUTED TOMOGRAPHY, AND ULTRASONIC EXAMINATIONS.
Sonography should ideally be used to confirm a clinically suspected breech presentation and to identify, if possible, any fetal anomalies. If cesarean delivery is planned, x-rays are not indicated. If, however, vaginal delivery is considered, the type of breech presentation is of considerable importance. Radiation exposure may be reduced considerably by using computed tomographic pelvimetry (Kopelman and associates, 1986). These imaging techniques can be used to provide information regarding the type of breech presentation, presence or absence of a flexed fetal head, and pelvic measurements.
The role of x-ray pelvimetry in deciding mode of delivery for breech presentation is controversial (Morrison and co-authors, 1995). Cheng and Hannah (1993) comprehensively surveyed the literature on breech delivery at term and reviewed 15 studies in which x-ray pelvimetry was used and 2 studies in which CT pelvimetry was used as one of the criteria for allowing vaginal delivery. They concluded that interpretation of the role of x-ray pelvimetry was complicated because pelvic dimensions for allowing labor varied among studies. Most authors, however, found no correlation between radiological pelvic measurements and the outcome of labor, while only one study (Ohlsén, 1975) demonstrated that the incidence of complicated labor rose with decreasing pelvic capacity.
Delivery presentation describes the way the baby (fetus) is positioned to come down the birth canal for delivery.
THE DELIVERY PROCESS
The delivery process is described in terms of fetal station, lie, attitude, and presentation.
Fetal station:
This is the relationship between the presenting part of the baby -- the head, shoulder, buttocks, or feet -- and two parts of the mother's pelvis called the ischial spines. Normally the ischial spines are the narrowest part of the pelvis. They are a natural measuring point for the delivery progress.
If the presenting part lies above the ischial spines, the station is reported as a negative number from -1 to -5 (each number is a centimeter). If the presenting part lies below the ischial spines, the station is reported as a positive number from +1 to +5. The baby is said to be "engaged" in the pelvis when it is even with the ischial spines at 0 station.
Fetal lie:
This is the relationship between the head to tailbone axis of the fetus and the head to tailbone axis of the mother. If the two are parallel, then the fetus is said to be in a longitudinal lie. If the two are at 90-degree angles to each other, the fetus is said to be in a transverse lie. Nearly all (99.5%) fetuses are in a longitudinal lie.
Fetal attitude:
The fetal attitude describes the relationship of the fetus' body parts to one another. The normal fetal attitude is commonly referred to as the fetal position. The head is tucked down to the chest, with arms and legs drawn in towards the center of the chest. Abnormal fetal attitudes may include a head that is extended back or other body parts extended or positioned behind the back. Abnormal fetal attitudes can increase the diameter of the presenting part as it passes through the pelvis, increasing the difficulty of birth.
Fetal presentation:
Cephalic (head-first) presentation:
Cephalic presentation is considered normal and occurs in about 97% of deliveries. There are different types of cephalic presentation, which depend on the fetal attitude.
Rarely, the fetus' head is extended back, and the chin, face, or forehead will present first depending on the degree of extension. This is a more difficult delivery, because this is not the smallest part of the fetus' head. It may result in a need for cesarean delivery.
A cesarean delivery may be recommended for any of the fetal positions other than cephalic.
Breech presentation:
Breech presentation is considered abnormal and occurs about 3% of the time. A complete breech presentation occurs when the buttocks present first, and both the hips and knees are flexed. A frank breech occurs when the hips are flexed so the legs are straight and completely drawn up toward the chest. Other breech positions occur when either the feet or knees come out first.
Shoulder presentation:
The shoulder, arm, or trunk may present first if the fetus is in a transverse lie. This type of presentation occurs less than 1% of the time. Transverse lie is more common with premature delivery or multiple pregnancies.
BIOMECHANISM OF LABOR IN BREECH PRESENTATION
I moment – the internal breech rotation. The breech rotates and the fetal intertrochanteric diameter from one of oblique size of the pelvic inlet to anteteroposterior size of the pelvic outlet.
II moment – the lateral flexion of the body. The anterior hip is stemmed against the pubic arc. By lateral flexion of the fetal body the posterior hip is forced over the anterior margin of the perineum. Then anterior hip is born.
III moment – the internal shoulders rotation. After the birth of the breech, there is the slight external rotation as a result of the descends and rotations of the shoulders. The shoulders rotates on the pelvic floor and diameter biacromialis occupies anteroposterior diameter of the pelvic outlet.
IV moment – the lateral flexion the body in the thoraco-brachial part. The shoulders are born.
V moment – the internal rotation of the head. The rotation begins when the fetal head descends from the plane of greatest pelvic dimensions to the least pelvic dimensions (midpelvis). The rotation is complete when the head reaches the pelvic floor, the sagittal suture is in the anteroposterior diameter of the pelvic outlet and the small fontanel is under the symphysis.
VI moment – the flexion of the fetal head. The head fixes with its fossa suboccipitalis to the inferior margin of symphysis pubis and flexes. The face, forehead, vertex, and occiput are born.
Figure Fetal head engages in left occipito-anterior position (top) then descends into mid-cavity and rotates to full occipito-anterior (bottom)
THE MANUAL AIDS IN BREECH PRESENTATIONS
The manual aid by Tsovyanov I in frank breech presentations.
The aim of the manual aid: to prepare the maternal ways to the delivery of the head and shoulders and to keep the normal attitude of the fetus.
In the frank breech presentation the fetus extremities are flexed at the hips and extended at the knees and thus the feet lie in close proximity to the head. The circumference of the thorax with the crossing on it arms and legs is larger than circumference of the head and the after-coming head deliveries easily.
The technique. The aid begins after the delivery of the buttocks. The obstetrician’s hands are applied over the buttocks, the thumbs placed on the fetus sacrum and other fingers on the legs. The doctor gently supports the legs to avoid its flexion. If the normal attitude of the fetus is keeping the head deliveries easy.
The classic manual aid on the labor in complete and incomplete breech presentation.
The aim of the classic manual aid: to help of the shoulders and the head delivery.
The classic manual aid begins when the lower angular of the anterior scapula became visible. There are 4 moments of the classic manual aid.
I moment – the delivery of the posterior arm. The posterior shoulder must be delivered first. The feet are grasped in one hand and drawn upward over the groin of the mother toward which the ventral surface of the fetus is directed; in this manner, leverage is exerted upon the posterior shoulder, which slides out over the perineal margin, usually followed by the arm and hand.
II and III moment – the external trunk rotation and the freeing the posterior arm. The aim of this moment is the reverse of the anterior shoulder to the sacrum and the delivery of second arm. The obstetrician applies his hand on the lateral sides of the fetus trunk and rotates it. The direction of the movement must be in this way: the occiput must go under the symphysis pubis. When the posterior shoulder and arm appears at the vulva the doctor put two fingers into the vagina, the fingers passed along the humorous until the elbow is reached. The fingers are now used to splint the arm, which is swept downward and delivered through the vulva.
IV moment – the freeing of the head. After the shoulder are born, the head usually occupies an oblique diameter of the pelvic with the occiput directed anteriorly. The fetal head may then be extracted by the method of Mauriceau-Levret. Employing the Mauriceau-Levre maneuver to help flex the head, the doctor’s middle finger of one hand are applied into the fetal mouth, while the fetal body rests upon the palm of the hand and fore arm, which is straddled the fetal legs. Two fingers of the operator’s other hand are then hooked over the fetal neck and grasping the shoulders, downward traction is applied until the suboccipital region appears under the symphysis. The body of the fetus is then elevated toward the mother abdomen, and the mouth, nose, brow and the occiput emerge over the perineum. Gentle traction should be exerted by the fingers over the shoulders.
The manual aid by Tsovyanov II in footling presentations.
The aim of the manual aid: To perform the footling presentation to the incomplete breech and to prepare the maternal ways to the delivery of the head and shoulders.
The doctor covers the area of the vulva with the sterile napkin and puts up resistance to the delivery of the feet. The feet are flexing and the footling presentation becomes incomplete breech presentation. Than the delivery manage as in incomplete breech presentation.
To try the minimize infant mortality and morbidity, cesarean section is now commonly used.
The indications to the cesarean section:
1. Breech presentation and a large fetus (the weight of the fetus estimated 3700 g and more).
2. Breech presentation and any degree of contraction or unfavorable shape of the pelvis.
3. Breech presentation and deflexed head.
4. Breech presentation and uterine dysfunction.
5. Breech presentation and previous perinatal death of children suffering from birth trauma.
6. Breech presentation and fetal hypoxia.
Prognosis. Both mother and fetus are at greater risk with breech presentation compared with cephalic presentation, but to nowhere near the same degree. In an analysis of 57,819 pregnancies in the Netherlands, Schutte and colleagues (1985) reported that even after correction for gestational age, congenital defects, and birthweight, perinatal mortality was higher in breech than in cephalic infants. They concluded that it may be possible that breech presentation is not coincidental but is a consequence of poor fetal quality. If this were true, then medical intervention may be unlikely to reduce perinatal mortality associated with breech presentation. This possibility had been suggested earlier by Hytten (1982) and by Susuki and Yamamuro (1985). This concept was strengthened by the report of Nelson and Ellenberg (1986), who observed that one third of children with cerebral palsy who were in a breech presentation at birth had major noncerebral malformations.
Because of the greater frequency of operative delivery, including cesarean delivery, there is a higher maternal morbidity and slightly higher mortality for pregnancies complicated by persistent breech presentation (Collea and co-authors, 1980). This risk is likely increased even more if an emergency operation is performed instead of an elective cesarean delivery (Bingham and Lilford, 1987). Labor is usually not prolonged; Hall and Kohl (1956) reported the median duration of labor to be 9.2 hours for nulliparas and 6.1 hours for multiparas.
The prognosis for the fetus in a cephalic presentation is considerably worse than when in a vertex presentation. The major contributors to perinatal loss are preterm delivery, congenital anomalies, and birth trauma. Brenner and associates (1974) provided a careful analysis of the characteristics and perils to the fetus from breech presentation. They determined the overall mortality rate for 1016 breech deliveries to be 25 percent compared with 2.6 percent for nonbreech deliveries at the University Hospitals of Cleveland. At every stage of gestation, they identified antepartum, intrapartum, and neonatal deaths to be significantly greater among breeches, and the average Apgar scores to be lower for those who survived. During the latter half of pregnancy, the birthweight at any gestational age was somewhat less for breech infants. Congenital abnormalities were identified in 6.3 percent of breech deliveries compared with 2.4 percent of nonbreech deliveries.
Tank and associates (1971) examined the character of serious traumatic vaginal delivery. At autopsy, the organs most frequently found to be injured were, in order of frequency, the brain, spinal cord, liver, adrenal glands, and spleen. It is of interest that, in retrospective analysis of cases of “idiopathic” adrenal calcification, breech delivery was very common. Other injuries from vaginal delivery included the brachial plexus; the pharynx, in the form of tears or pseudodiverticula from the obstetrician’s finger in the mouth as part of the Mauriceau maneuver; and the bladder, which might be ruptured if distended. Traction might injure the sternocleidomastoid muscle and, if not appropriately treated, lead to torticollis.
PROBLEMS WITH VAGINAL DELIVERY
Delivery of the breech draws the umbilicus and attached cord into the pelvis, which compresses the cord. Therefore, once the breech has passed beyond the vaginal introitus, the abdomen, thorax, arms, and head must be delivered promptly. This involves delivery of successively less readily compressible parts. With a term fetus, some degree of head molding may be essential for it to negotiate the birth canal successfully. In this unfortunate circumstance, the alternatives with vaginal delivery are both unsatisfactory: (1) delivery may be delayed many minutes while the aftercoming head accommodates to the maternal pelvis, but hypoxia and acidemia become severe; or (2) delivery may be forced, causing trauma from compression, traction, or both.
With a preterm fetus, the disparity between the size of the head and buttocks is even greater than with a larger fetus. At times, the buttocks and lower extremities of the preterm fetus will pass through the cervix and be delivered, and yet the cervix will not be dilated adequately for the head to escape without trauma (Bodmer and associates, 1986). In this circumstance, Dührssen incisions of the cervix may be attempted. Even so, trauma to the fetus and mother may be appreciable, and fetal hypoxia may prove harmful. Another mechanical problem with breech delivery is entrapment of the fetal arm behind the neck. A nuchal arm complicates up to 6 percent of vaginal breech deliveries and is associated with increased neonatal mortality (Cheng and Hannah, 1993).
The frequency of cord prolapse is increased when the fetus is small or when the breech is not frank. In the report by Collea and colleagues (1978), the incidence with frank breech presentation was about 0.5 percent, which is similar to the incidence (0.4 percent) reported for cephalic presentations (Barrett, 1991). In contrast, the incidence of cord prolapse with footling presentation was 15 percent, and it was 5 percent with complete breech presentation.
Soernes and Bakke (1986) confirmed earlier observations that the umbilical cord length is significantly shorter in breech compared with cephalic presentations. Moreover, multiple coils of cord entangling the fetus are more common in breech presentations (Spellacy and associates, 1966). These umbilical cord abnormalities likely play a role in the development of breech presentation as well as the relatively high incidence of a non-reassuring fetal heart rate pattern in labor. For example, Flanagan and co-workers (1987) selected 244 women with a variety of breech presentations (72 percent were frank breech) for a trial of labor, and there was a cord prolapse in 4 percent. Fetal distress not due to cord prolapse was diagnosed in another 5 percent of women selected for vaginal delivery. Overall, 10 percent of the women identified for vaginal birth underwent cesarean deliveries for fetal jeopardy in labor.
Apgar scores, especially at 1 minute, of vaginally delivered breech infants are generally lower than when elective cesarean delivery is performed (Flanagan and co-workers, 1987). Similarly, neonatal cord blood acid–base values are significantly different for vaginally delivered breech infants. Christian and Brady (1991) reported that umbilical artery blood pH was lower, PCO2 higher, and HCO3 lower compared with cephalic deliveries. Socol and colleagues (1988), however, concluded that cesarean delivery improved Apgar scores but not acid–base status. Flanagan and co-workers (1987) emphasized that ultimate infant outcome for breech birth was not worsened by these significant differences in Apgar scores or acid–base status at birth.
Unfavorable Pelvis. Because there is no time for molding of the aftercoming head, a moderately contracted pelvis that had not previously caused problems in delivery of an average-size cephalic fetus might prove dangerous with a breech. Rovinsky and colleagues (1973) urged not only accurate measurements of the pelvic dimensions but also precise evaluation of the pelvic architecture rather than reliance on pelvic indexes. Gynecoid (round) and anthropoid (elliptical) pelves are favorable configurations, but platypelloid (anteroposteriorly flat) and android (heart-shaped) pelves are not.


Fig. 6. Hyperextension of Fetal Head
In perhaps 5 percent of term breech presentations, the fetal head may be in extreme hyperextension (Fig. 19). In these, vaginal delivery may result in injury to the cervical spinal cord. In general, marked hyperextension after labor has begun is considered an indication for cesarean delivery (Svenningsen and associates, 1985).
Induction of labor in women with a breech presentation is defended by some and condemned by others. Brenner and associates (1974) found no significant differences in mortality rates and Apgar scores between cases with induced and those with spontaneous labor. In oxytocin-augmented labor, however, infant mortality rates were higher, and Apgar scores were lower. Gimovsky and Paul (1982) observed that augmentation of labor was followed by vaginal delivery in only 2 of 9 women, both multiparous. Moreover, one of the two deliveries resulted in entrapment of the aftercoming fetal head. The general policy at Parkland Hospital is to resort to cesarean delivery, rather than use oxytocin to induce or augment labor, unless the fetus is previable or has a severe anomaly.
The possibility of compression of a prolapsed cord or a cord entangled around the extremities as the breech fills the pelvis, if not before, is a threat to the fetus.
With a preterm fetus, the aftercoming head may be trapped by a cervix that is sufficiently effaced and dilated to allow passage of the thorax but not the less compressible head. The consequences of vaginal delivery in this circumstance all too often have been both hypoxia and physical trauma, both of which are especially deleterious to the preterm infant. Thus, delivery of the apparently healthy but very small fetus by cesarean is generally recommended.
Cheng and Hannah (1993) conducted a systemic search of the world literature regarding term breech delivery and found 82 reports published in English between 1966 and 1992. A total of 24 studies were selected for analysis because these compared planned vaginal delivery with planned cesarean section for the term, singleton breech fetus. The effects of planned vaginal delivery on perinatal mortality, corrected for lethal congenital anomalies and antepartum fetal death. The corrected perinatal mortality rate ranged from 0 to 48 per 1000 births and was higher among infants in the planned vaginal delivery groups.
All but two deaths were in the groups of women allowed to labor and deliver vaginally. The main causes of death were head entrapment, cerebral injury and hemorrhage, cord prolapse, and severe asphyxia. Cheng and Hannah (1993) observed that the overall neonatal mortality and morbidity resulting from trauma were increased significantly in the planned vaginal delivery groups, with a typical odds ratio of 3.86. They suggested that until a well-designed randomized trial with sufficient statistical power is performed, planned cesarean delivery should be strongly considered for persistent breech presentation at term. Similarly, Gifford and co-workers (1995) performed a meta-analysis of outcomes after term breech delivery and observed that, given many methodological limitations of published studies, their analysis suggested an increased risk of injury or death after a trial of labor.
Only 2 of the 24 reports reviewed by Cheng and Hannah (1993) and Gifford and co-workers (1995) were randomized trials, and both were from the same institution. Collea and colleagues (1980) reported the results of 200 women with frank breech fetuses at term. Almost half of these women were excluded from further consideration because of possible fetopelvic disproportion based on x-ray pelvimetry. A total of 60 infants were eventually delivered vaginally, and all survived, although two sustained brachial plexus injuries. There were no perinatal deaths, but half of the 148 women who had cesarean deliveries experienced significant morbidity compared with only 7 percent of 60 women who were delivered vaginally. Gimovsky and colleagues (1983) later evaluated 105 nonfrank breech fetuses and reported similar findings. Although these two trials concluded that vaginal breech delivery was relatively safe, only 110 fetuses were actually allowed a trial of labor after careful selection. As emphasized by Eller and Van Dorsten (1995), this small number would not provide sufficient statistical power to demonstrate differences in uncommon adverse outcomes such as perinatal death and birth injury.
There are no randomized studies regarding delivery of the preterm breech fetus. Penn and colleagues (1996) attempted such a study in 26 hospitals in England and discontinued the trial after 17 months because only 13 patients could be recruited. Retrospective studies have yielded conflicting results. Bowes and colleagues (1979) and Main and co-workers (1983) found that infants born by cesarean section had a better prognosis. Others concluded that vaginal delivery did not significantly increase perinatal mortality (Olshan and co-workers, 1984; Rosen and Chik, 1984; Westgren and co-workers, 1985a, c). The National Institute of Child Health and Human Development Neonatal Research Network (Malloy and co-workers, 1991) collected data on 437 very-low-birthweight breech infants admitted to seven neonatal intensive care centers. After adjusting for several variables, the risk of intraventricular hemorrhage and neonatal death was not significantly affected by the mode of delivery for breech fetuses weighing less than 1500 g. A similar analysis was reported from the Netherlands (Gravenhorst and co-workers, 1993). Perinatal follow-up data were collected on 899 live-born singleton, nonanomalous infants with gestational age less than 32 weeks and birthweight less than 1500 g. Statistical analysis failed to conclusively resolve whether cesarean delivery was advantageous.
Eller and Van Dorsten (1995) recently surveyed the centers in the Maternal–Fetal Medicine Units Network to determine the feasibility of resolving the controversy regarding route of delivery by a randomized clinical trial. Virtually all participating obstetricians in the Network agreed that clear scientific evidence was needed to determine if mode of delivery of the breech affects outcome. Performing the needed investigation was judged to be not feasible, however, because the number of skilled operators with the ability to safely deliver breech fetuses continues to dwindle and medicolegal concerns make it difficult to train residents to perform such deliveries. Indeed, at least two other groups of investigators, who have attempted trials of breech delivery, concluded that such studies were likely impossible (Penn and Steer, 1990; Zlatnik, 1993).
What then is “standard of
care” for delivery of term and preterm singleton breech presentations in the United
States? Despite the inadequacy of scientific evidence as discussed, most breech
presentations are delivered by cesarean section. Green and colleagues (1982)
estimated that about 90 percent of breech presentations of all gestational ages
undergo cesarean delivery. There are centers in the United States, however, in
which perhaps half of breech presentations are safely delivered vaginally. For
example, 44 percent of breeches weighing 1500 g or more and 60 percent of those less than 1500 g are safely delivered vaginally at the Chicago Lying-in Hospital
(Brown and co-authors, 1994; Cibils and colleagues, 1994). At Parkland
Hospital, the route of delivery is individualized to clinical circumstances by
the attending faculty physician. Women with selected frank breech presentations
of about 2000 g or more but less than about 3500 g are frequently offered planned vaginal delivery. Nonetheless, 85 percent of all singleton
breech presentations in 1995 were delivered by cesarean section. We are of the
view that individualized cesarean or vaginal delivery are both reasonable and
acceptable in current obstetrical practice. 
|
|
Media file 2: Assisted vaginal breech delivery. Thick meconium passage is common as the breech is squeezed through the birth canal. This is usually not associated with meconium aspiration because the meconium passes out of the vagina and does not mix with the amniotic fluid. |
|
|
Media file 3: Assisted vaginal breech delivery. The Ritgen maneuver is applied to take pressure off the perineum during vaginal delivery. Episiotomies are often performed for assisted vaginal breech deliveries, even in multiparous women, to prevent soft tissue dystocia. |
|
|
Media file 4: Assisted vaginal breech delivery. No downward or outward traction is applied to the fetus until the umbilicus has been reached. |
|
|
Media file 5: Assisted vaginal breech delivery. With a towel wrapped around the fetal hips, gentle downward and outward traction is applied in conjunction with maternal expulsive efforts until the scapula is reached. An assistant should be applying gentle fundal pressure to keep the fetal head flexed. |
|
|
Media file 6: Assisted vaginal breech delivery. After the scapula is reached, the fetus should be rotated 90° in order to deliver the anterior arm. |
|
|
Media file 7: Assisted vaginal breech delivery. The anterior arm is followed to the elbow, and the arm is swept out of the vagina. |
|
|
Media file 8: Assisted vaginal breech delivery. The fetus is rotated 180°, and the contralateral arm is delivered in a similar manner as the first. The infant is then rotated 90° to the backup position in preparation for delivery of the head. |
|
|
Media file 9: Assisted vaginal breech delivery. The fetal head is maintained in a flexed position by using the Mauriceau maneuver, which is performed by placing the index and middle fingers over the maxillary prominence on either side of the nose. The fetal body is supported in a neutral position, with care to not overextend the neck. |
|
|
Media file 10: Piper forceps application. Piper forceps are specialized forceps used only for the after-coming head of a breech presentation. They are used to keep the fetal head flexed during extraction of the head. An assistant is needed to hold the infant while the operator gets on one knee to apply the forceps from below. |
|
|
Media file 11: Assisted vaginal breech delivery. Low 1-minute Apgar scores are not uncommon after a vaginal breech delivery. A pediatrician should be present for the delivery in the event that neonatal resuscitation is needed. |
|
|
Media file 13: Ultrasound demonstrating a fetus in breech presentation with a hyperextended head (ie, "star gazing"). |
EXTERNAL CEPHALIC VERSION
Whenever a breech presentation is recognized during the third trimester, an attempt may be made to substitute a cephalic presentation by external version. This procedure, well known to our obstetrical predecessors, has received renewed interest in the past two decades coincidental with the availability of ultrasound, electronic fetal monitoring, and effective tocolytic agents. It is likely that these developments have improved the maternal and fetal safety of external version compared with prior obstetrical eras.
Van Dorsten and co-workers (1981) rekindled interest in this procedure in the United States. They used ultrasound, fetal monitoring, and a b-agonist for uterine relaxation in 25 pregnancies randomized to receive external version between 37 and 39 weeks and compared outcomes with 23 similar pregnancies managed without version. Almost 70 percent of versions were successful, resulting in a 30 percent cesarean delivery rate compared with 75 percent when version was not attempted. It is estimated that an active program of breech version could reduce the expected 3 to 4 percent breech presentation rate at delivery by about half (Laros and colleagues, 1995).

Fig. 7 Hypothetical results of a trial of external cephalic version for breech presentation derived from 1339 published patients. (From Zhang J, Bowes WA, Fortney JA. Efficacy of external cephalic version: A review. Obstet Gynecol. 82:306, 1993. Modified with permission from the American College of Obstetricians and Gynecologists.
Can a breech presentation be changed?
It is preferable to try to turn a breech baby between the 32nd and 37th weeks of pregnancy. The methods of turning a baby will vary and the success rate for each method can also vary. It is best to discuss the options with the health care provider to see which method he/she recommends.
Medical Techniques:
External Version: External version is a non-surgical technique to move the baby in the uterus. In this procedure, a medication is given to help relax the uterus. There might also be the use of ultrasound to determine the position of the baby, the location of the placenta and the amount of amniotic fluid in the uterus. Gentle pushing on the lower abdomen can turn the baby into the head-down position. Throughout the external version the baby’s heartbeat will be closely monitored so that if a problem develops, the health care provider will immediately stop the procedure. External version has a high success rate. However, this procedure becomes more difficult as the due date gets closer.
Chiropractic Care: The late Larry Webster, D.C., of the International Chiropractic Pediatric Association, developed a technique that enabled chiropractors to reduce stress on the pregnant woman’s pelvis leading to the relaxation of the uterus and surrounding ligaments. A more relaxed uterus makes it easier for a breech baby to turn naturally. His technique is known as the Webster Breech Technique.
The July/August issue of the Journal of Manipulative and Physiological Therapeutics reported and 82% success rate for the Webster Technique. Further, the results of the study suggest that it is preferable to perform the Webster Technique in the 8th month of pregnancy.
Natural Techniques:
The following risk-free techniques, often suggested by physical therapist, Penny Simkin, can be tried at home for free:
The Breech Tilt: Using large, firm pillows, raise the hips 12″ or 30cm off the floor for 10-15 minutes, three times a day. It is best to do this on an empty stomach when your baby is active. In this technique, try to concentrate on the baby without tensing your body, especially in the abdominal area.
Using Music: We know that babies can hear sounds outside the womb. Consequently, many women have used music or taped recordings of their voice to try to get their baby to move towards the sound! Placing headphones on the lower part of your abdomen and playing either music or sounds of your voice can encourage babies to move towards the sounds and out of a breech position.
Some homeopathic remedies have also been found to be successful in correcting breech positions. If interested, you can contact your local holistic practitioner about the possibility of using of Moxibustion or Pulsatilla to correct a breech position.
Vaginal delivery versus cesarean for breech birth?
Most health care providers do not believe in attempting a vaginal delivery for a breech position. However, some will delay making a final decision until the woman is in labor. The following conditions are considered necessary in order to attempt a vaginal birth:
· The baby is full-term and in the frank breech presentation
.
· The baby does not show signs of distress while its heart rate is closely monitored.
· The process of labor is smooth and steady with the cervix widening as the baby descends.
· The health care provider estimates that the baby is not too big or the mother’s pelvis too narrow for the baby to pass safely through the birth canal.
· Anesthesia is available and a cesarean delivery possible on short notice
What are the risks and complications of a vaginal delivery?
In a breech birth, the baby’s head is the last part of its body to emerge making it more difficult to ease it through the birth canal. Sometimes forceps are used to guide the baby’s head out of the birth canal. Another potential problem iscord prolapse. In this situation the umbilical cord is squeezed as the baby moves toward the birth canal, thus slowing the baby’s supply of oxygen and blood.
In a vaginal breech delivery, electronic fetal monitoring will be used to monitor the baby’s heartbeat throughout the course of labor. A cesarean delivery may be an option if signs develop that the baby may be in distress.
When is a cesarean delivery used with a breech presentation?
Most health care providers recommend a cesarean delivery for all babies in a breech position, especially babies that are premature. Since premature babies are small and more fragile, and because the head of a premature baby is relatively larger in proportion to its body, the baby is unlikely to stretch the cervix as much as a full-term baby. This means that there might be less room for the head to emerge.
Zhang and co-authors (1993) reviewed 25 selected reports on external cephalic version published between 1980 and 1991. Shown in Figure 20, and based on data derived from their review, are hypothetical results if all women with otherwise normal pregnancies and with singleton breech presentations had attempted external cephalic version at 35 to 37 weeks. Several points are noteworthy: (1) external cephalic version is successful in 65 percent of cases; (2) if version succeeds, almost all fetuses stay in the cephalic presentation, and vice-versa; and (3) ultimately, and despite version attempts, 37 percent of women identified to have late pregnancy breech presentations will require cesarean delivery. Zhang and co-workers (1993) estimated that universal application of external cephalic version could reduce the overall cesarean rate by no more than 2 percent.
PROCEDURE


From 30-32 weeks -correcting gymnastics in breech presentations



Prepare for the possibility of cesarean delivery. Obtain a type as well as an anesthesia consult. The patient should have nothing by mouth for at least 8 hours prior to the procedure. Perform an ultrasound to confirm breech, check growth and amniotic fluid volume, and rule out anomalies associated with breech.
Perform a nonstress test (biophysical profile as backup) prior to ECV to confirm fetal well-being.
Perform ECV in or near a delivery suite in the unlikely event of fetal compromise during or following the procedure, which may require emergent delivery.
ECV can be performed with 1 or 2 operators. An assistant may help turn the fetus, elevate the breech out of the pelvis, or monitor the ultrasound position of the baby.
ECV is accomplished by judicious manipulation of the fetal head toward the pelvis while the breech is brought up toward the fundus. Attempt a forward roll first and then a backward roll if the initial attempts are unsuccessful. No consensus has been reached regarding how many ECV attempts are appropriate at one time.
Following an ECV attempt, whether successful or not, repeat the nonstress test (biophysical profile if needed) prior to discharge. Also, administer Rh immune globulin to women who are Rh-negative. Some physicians induce labor following successful ECV. However, as virtually all of these recently converted fetuses are unengaged, many practitioners will discharge the patient and wait for spontaneous labor to ensue, thereby avoiding the risk of a failed induction of labor.
In those with an unsuccessful ECV, the practitioner has the option of sending the patient home or proceeding with a cesarean delivery. Expectant management allows for the possibility of spontaneous version. Alternatively, cesarean delivery may be performed at the time of the failed ECV, especially if regional anesthesia is used (see Regional anesthesia). This would minimize the risk of a second regional analgesia. However, be aware of the small risk for iatrogenic respiratory distress syndrome, especially when delivery is prior to 37 weeks' gestation.
SUCCESS RATE
Success rates vary widely but range from 35-86% (average, 58%). Improved success rates occur with multiparity, with earlier gestational age, with frank breech presentation, with a transverse lie, and in African American patients. Opinions differ regarding the influence of maternal weight, placental position, and amniotic fluid volume, but these factors may also influence success rates. Be prepared for an unsuccessful ECV; version failure is not necessarily a reflection of the skill of the practitioner.
Zhang reviewed 25 studies of ECV in the United States, Europe, Africa, and Israel. The average success rate in the United States was 65%. Of successful ECVs, 2.5% reverted to breech presentation (other estimates range from 3-5%, while 2% of unsuccessful ECVs had spontaneous version to cephalic presentation (other estimates range from 12-26%) prior to labor. Spontaneous version rates depend on the gestational age when the breech is discovered, with earlier breeches more likely to have spontaneous version.
The performance of an ECV decreases the cesarean delivery rate for breech by approximately 50%. Because breech presentations complicate only 3-5% of all deliveries, decreasing the cesarean delivery rate for breeches by 50% will have only a marginal impact on the overall cesarean delivery rate.
Hofmeyr and Kulier reviewed 5 randomized clinical trials of ECV versus no ECV at term. ECV was associated with a significant reduction in noncephalic births (relative risk [RR], 0.38; 95% confidence interval [CI], 0.18-0.8) and a reduction in cesarean delivery for breech (RR, 0.55; 95% CI, 0.33-0.91).
While most studies of ECV have been performed in university hospitals, Cook showed that ECV has also been effective in the private practice setting. Of 65 patients with term breeches, 60 were offered ECV. ECV was successful in 32 (53%) of the 60 patients, with vaginal delivery in 23 (72%) of the 32 patients. Of the remaining breech fetuses believed to be candidates for vaginal delivery, 8 (80%) had successful vaginal delivery. The overall vaginal delivery rate was 48% (31 of 65 patients), with no significant morbidity.
COST ANALYSIS
In 1995, Gifford et al performed a cost analysis of 4 options for breech presentations at term: (1) ECV attempt on all breeches, with attempted vaginal breech delivery for selected persistent breeches; (2) ECV on all breeches, with cesarean delivery for persistent breeches; (3) trial of labor for selected breeches, with scheduled cesarean delivery for all others; and (4) scheduled cesarean delivery for all breeches prior to labor.
ECV attempt on all breeches with attempted vaginal breech delivery on selected persistent breeches was associated with the lowest cesarean delivery rate and was the most cost-effective approach. The second most cost-effective approach was ECV attempt on all breeches, with cesarean delivery for persistent breeches.
RISKS
Uncommon risks of ECV include fractured fetal bones, precipitation of labor or premature rupture of membranes, abruptio placentae, fetomaternal hemorrhage (0-5%), and cord entanglement ( <1.5%). A more common risk of ECV is transient slowing of the fetal heart rate (in as many as 40% of cases). This risk is believed to be a vagal response to head compression with ECV. It usually resolves within a few minutes after cessation of the ECV attempt and is not usually associated with adverse sequelae for the fetus.
Women with breech presentation, reassuring fetal heart rate tracings, and no contraindications to vaginal delivery at 36 weeks' gestation and beyond are usually candidates for ECV (see Contraindications below).
ECV is usually not performed on preterm breeches because they are more likely to undergo spontaneous version to cephalic presentation and are more likely to revert to breech after successful ECV (approximately 50%). Studies of preterm ECV did not show a difference in the rates of breech presentations at term or overall rates of cesarean delivery. Additionally, if complications of ECV were to arise that warranted emergent delivery, it would result in a preterm neonate with its inherent risks.
CONTRAINDICATIONS
Absolute contraindications for ECV include multiple gestations with a breech presenting fetus, contraindications to vaginal delivery (eg, herpes simplex virus infection, placenta previa), and nonreassuring fetal heart rate tracing.
Relative contraindications include polyhydramnios or oligohydramnios, fetal growth restriction, uterine malformation, and fetal anomaly.
CONTROVERSIAL CANDIDATES
Women with prior uterine incisions may be candidates for ECV, but data are scant. In 1991, Flamm et al attempted ECV on 56 women with one or more prior low transverse cesarean deliveries. The success rate of ECV was 82%, with successful vaginal births in 65% of patients with successful ECVs. No uterine ruptures occurred during attempted ECV or subsequent labor, and no significant fetal complications occurred.
Another controversial area is performing ECV on a woman in active labor. In 1985, Ferguson and Dyson reported on 15 women in labor with term breeches and intact membranes. Four patients were dilated greater than 5 cm (2 women were dilated 8 cm). Ritodrine was used for acute tocolysis, and intrapartum ECV was attempted. ECV was successful in 11 of 15 patients, with successful vaginal births in 10 patients. No adverse effects were noted. Further studies are needed to evaluate the safety and efficacy of intrapartum ECV.
TOCOLYTICS
Data regarding the benefit of intravenous or subcutaneous beta-mimetics in improving ECV rates are conflicting.
In 1996, Marquette et al performed a prospective, randomized, double-blinded study on 283 subjects with breech presentations between 36 and 41 weeks' gestation. Subjects received either intravenous ritodrine or a placebo. The success rate of ECV was 52% in the ritodrine group versus 42% in the placebo group (P = .35). When only nulliparous subjects were analyzed, significant differences were observed in the success of ECV (43% vs 25%, P <.03). ECV success rates were significantly higher in parous versus nulliparous subjects (61% vs 34%, P <.0001), with no additional improvement with ritodrine.
In 2004, Hofmeyr reviewed 6 trials of tocolysis prior to ECV and concluded that routine tocolysis resulted in fewer failures of ECV (RR, 0.74; 95% CI, 0.64-0.87). Sublingual nitroglycerine was not found to be useful.
Whether tocolysis should be used routinely or selectively is still unclear.
REGIONAL ANESTHESIA
Regional analgesia, either epidural or spinal, may be used to facilitate ECV success. When analgesia levels similar to that for cesarean delivery are given, it allows relaxation of the anterior abdominal wall, making palpation and manipulation of the fetal head easier. Epidural or spinal analgesia also eliminates maternal pain that may cause bearing down and tensing of the abdominal muscles. If ECV is successful, patients can be induced with the epidural in place or the epidural can be removed and the patient sent home to await spontaneous labor. If ECV is unsuccessful, a patient can proceed to cesarean delivery under her current anesthesia.
The main disadvantage is the inherent risk of regional analgesia, which is considered small. Additionally, lack of maternal pain could potentially result in excessive force being applied to the fetus without the knowledge of the operator.
In 1994, Carlan et al retrospectively analyzed 61 women who were at more than 36 weeks' gestation and had ECV with or without epidural. The success rate of ECV was 59% in the epidural group and 24% in the nonepidural group (P <.05). In 7 of 8 women with unsuccessful ECV without epidural, a repeat ECV attempt after epidural was successful. Of the epidural group, 86% had obstetrical intervention (induction or cesarean delivery) immediately after the ECV. No effects on maternal or perinatal morbidity or mortality occurred.
In 1997, Schorr et al randomized 69 subjects who were at least 37 weeks' gestation to either epidural or control groups prior to attempted ECV. Those in whom ECV failed underwent cesarean delivery. The success rate of ECV was 69% in the epidural group and 32% in the control group (RR, 2.12; 95% CI, 1.24-3.62). The cesarean delivery rate was 79% in the control group and 34% in the epidural group (P = .001). No complications of epidural anesthesia and no adverse fetal effects occurred.
In 1999, Dugoff et al randomized 102 breech subjects who were at more than 36 weeks' gestation with breech presentations to either spinal anesthesia or a control group. All subjects received 0.25 mg terbutaline subcutaneously. The success rate of ECV was 44% in the spinal group and 42% in the nonspinal group, which was not statistically significant.
It would hence appear that epidural analgesia, though not spinal, is associated with a higher success rate of ECV. Further studies are needed to confirm these initial findings.
ACOUSTIC STIMULATION
Johnson and Elliott performed a randomized, blinded crossover trial on 23 subjects to compare acoustic stimulation prior to ECV with a control group when the fetal spine was in the midline (directly back up or back down). Of those who received acoustic stimulation, 12 of 12 fetuses shifted to a spine-lateral position after acoustic stimulation, and 11 (91%) underwent successful ECV. In the control group, 0 of 11 shifts and 1 (9%) successful ECV (P <.0001) occurred. After crossover to the alternate modality, all 10 fetuses in the control group in whom ECV initially failed shifted to a spine-lateral position following acoustic stimulation and 8 of these had successful ECV, compared with 0 of 1 ECV successes in the acoustic stimulation group that crossed over to the control group.
VAGINAL DELIVERY RATES AFTER SUCCESSFUL VERSION
The rate of cesarean delivery ranges from 0-31% after successful ECV.
In 1994, a retrospective study by Egge et al of 76 successful ECVs matched with cephalic controls by delivery date, parity, and gestational age failed to note any significant difference in the cesarean delivery rate (8% in ECV group, 6% in control group).
In 1997, Lau et al compared 154 successful ECVs to 308 spontaneously occurring cephalic controls (matched for age, parity, and type of labor onset) with regard to the cesarean delivery rate. Cesarean delivery rates were higher after ECV (16.9% vs 7.5%, P <.005) because of higher rates of cephalopelvic disproportion and nonreassuring fetal heart rate tracings. This may be related to an increased frequency of compound presentations after ECV.
Immediate induction of labor after successful ECV may also contribute to an increase in the cesarean delivery rate due to failed induction in women with unripe cervices and unengaged fetal heads.
Vaginal breech delivery requires an experienced obstetrician and careful counseling for the parent(s). Although studies on the delivery of the preterm breech are limited, the recent multicenter term breech trial found an increased rate of perinatal mortality and serious immediate perinatal morbidity.
Parents must be informed about potential risks and benefits to the mother and neonate for both vaginal breech delivery and cesarean delivery. The likelihood is high that the trend will continue toward 100% cesarean delivery for term breeches and that vaginal breech deliveries will no longer be performed.
ECV is a safe alternative to vaginal breech delivery or cesarean delivery, reducing the cesarean delivery rate for breech by 50%. The ACOG, in its 2000 Practice Bulletin, recommends offering ECV to all women with a breech fetus near term. Consider adjuncts such as tocolysis, regional anesthesia, and acoustic stimulation to improve ECV success rates. Before performing a delivery or ECV on a mother whose fetus is in a breech presentation, assess for any underlying fetal abnormalities or uterine conditions that may result in a malpresentation
FACTORS ASSOCIATED WITH SUCCESSFUL VERSION
The most consistent factor associated with the success of external cephalic version is parity (Zhang and colleagues, 1993). Gestational age is also important; the earlier external version is performed, the more likely it will be successful. Conversely, the more remote from term external version is performed, the higher the rate of spontaneous reversion (Westgren and colleagues, 1985b). Other reported, albeit controversial, determinants of unsuccessful version include diminished amnionic fluid volume, excessive maternal weight, anterior placental location, cervical dilatation, descent of the breech into the pelvis, and anterior or posterior positioning of the fetal spine (Newman and colleagues, 1993, Zhang and co-authors, 1993). Remarkably, Johnson and Elliott (1995) used fetal acoustic stimulation to startle breech fetuses to shift their spines laterally for successful external version! Fernandez and co-workers (1996) randomized 103 women with term antepartum singleton breech presentations to receive terbutaline 250 mg subcutaneously or placebo. Use of terbutaline significantly enhanced the success of external cephalic version from 27 to 52 percent. Marquette and colleagues (1996) reported similar results using ritodrine infusions.
Women with a transverse lie are usually excluded from analyses of breech version because the overall success rate approaches 90 percent (Newman and colleagues, 1993).
TECHNIQUE
External cephalic version is typically carried out in a labor and delivery unit (Newman and colleagues, 1993), although Kornman and colleagues (1995) have performed selected versions in an office setting. Real-time ultrasonic examination is performed to confirm nonvertex presentation, the adequacy of amnionic fluid volume (vertical pocket of 2 cm or greater), fetal measurements consistent with term gestation, and estimated fetal weight; to rule out obvious fetal anomalies; and to identify placental location. A nonstress test is performed to assess fetal heart rate reactivity. Terbutaline sulfate, 250 mg, is given subcutaneously and version attempted 20 minutes later. “Forward roll” of the fetus is usually attempted first and the “back flip” technique is then tried if unsuccessful. Version attempts are discontinued for excessive discomfort, persistently abnormal fetal heart rate, or after multiple failed attempts. D-immune globulin is given to D-negative, unsensitized women. The nonstress test is repeated after the version until a normal test result is obtained. This process takes about half a day and may cost as much as $1700 (Newman and colleagues, 1993).
According to Zhang and colleagues (1993), there have been no reported fetal deaths in the United States resulting directly from external version since 1980. Reported nonfatal complications include fetal heart rate decelerations in almost 40 percent of fetuses (Phelan and co-workers, 1984) and fetomaternal hemorrhage in 4 percent (Stine and colleagues, 1985). Petrikovsky and colleagues (1987) reported a case of fetal brachial plexus injury after a successful external version. Stine and co-workers (1985) reported a maternal death due to amnionic fluid embolus.
MALPOSITIONS AND MALPRESENTATIONS
Malpositions are abnormal positions of the vertex of the fetal head (with the occiput as the reference point) relative to the maternal pelvis. Malpresentations are all presentations of the fetus other than vertex.
PROBLEM
· The fetus is in an abnormal position or presentation that may result in prolonged or obstructed labour.
GENERAL MANAGEMENT
· Make a rapid evaluation of the general condition of the woman including vital signs (pulse, blood pressure, respiration, temperature).
· Assess fetal condition:
- Listen to the fetal heart rate immediately after a contraction:
- Count the fetal heart rate for a full minute at least once every 30 minutes during the active phase and every 5 minutes during the second stage;
- If there are fetal heart rate abnormalities (less than 100 or more than 180 beats per minute), suspect fetal distress.
- If the membranes have ruptured, note the colour of the draining amniotic fluid:
- Presence of thick meconium indicates the need for close monitoring and possible intervention for management of fetal distress;
- Absence of fluid draining after rupture of the membranes is an indication of reduced volume of amniotic fluid, which may be associated with fetal distress.
· Provide encouragement and supportive care.
· Review progress of labour using a partograph.
Note: Observe the woman closely. Malpresentations increase the risk for uterine rupture because of the potential for obstructed labour.
DIAGNOSIS
DETERMINE THE PRESENTING PART
· The most common presentation is the vertex of the fetal head. If the vertex is not the presenting part, see Table S-12.
|
Symptoms and Signs |
Figure |
|
BROW PRESENTATION is caused by partial extension of the fetal head so that the occiput is higher than the sinciput (Fig S-16). On abdominal examination, more than half the fetal head is above the symphysis pubis and the occiput is palpable at a higher level than the sinciput. On vaginal examination, the anterior fontanelle and the orbits are felt. |
FIGURE S-16 |
|
FACE PRESENTATION is caused by hyper-extension of the fetal head so that neither the occiput nor the sinciput are palpable on vaginal examination (Fig S-17 and Fig S-18). On abdominal examination, a groove may be felt between the occiput and the back. On vaginal examination, the face is palpated, the examiner’s finger enters the mouth easily and the bony jaws are felt. |
FIGURE S-17 FIGURE S-18 |
|
COMPOUND PRESENTATION occurs when an arm prolapses alongside the presenting part. Both the prolapsed arm and the fetal head present in the pelvis simultaneously (Fig S-19). |
FIGURE S-19 |
|
BREECH PRESENTATION occurs when the buttocks and/or the feet are the presenting parts. On abdominal examination, the head is felt in the upper abdomen and the breech in the pelvic brim. Auscultation locates the fetal heart higher than expected with a vertex presentation. On vaginal examination
during labour, the buttocks and/or feet are felt; thick, dark meconium is
normal.
occurs when both legs are flexed at the hips and knees (Fig S-20). FRANK (EXTENDED) BREECH
PRESENTATION
FOOTLING BREECH PRESENTATION occurs when a leg is extended at the hip and the knee (Fig S-22). |
FIGURE S-20 FIGURE S-21 FIGURE S-22 |
|
TRANSVERSE LIE AND SHOULDER PRESENTATION occur when the long axis of the fetus is transverse (Fig S-23). The shoulder is typically the presenting part. On abdominal examination, neither the head nor the buttocks can be felt at the symphysis pubis and the head is usually felt in the flank. On vaginal examination, a shoulder may be felt, but not always. An arm may prolapse and the elbow, arm or hand may be felt in the vagina. |
FIGURE S-23 |
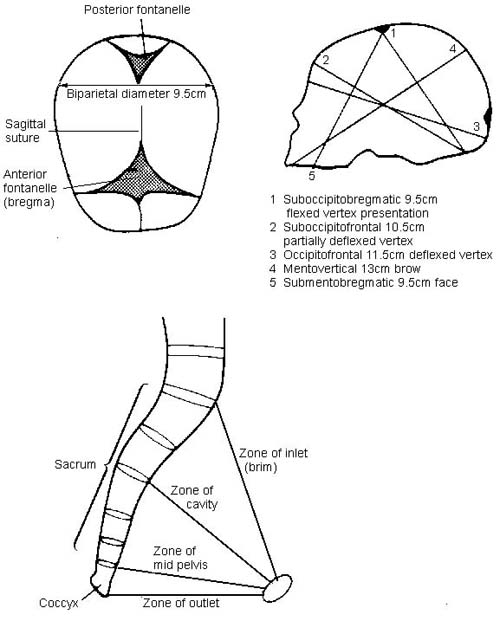
· If the vertex is the presenting part, use landmarks of the fetal skull to determine the position of the fetal head (Fig 9).
Figure 9 Landmarks of the fetal skull

DETERMINE THE POSITION OF THE FETAL HEAD
· The fetal head normally engages in the maternal pelvis in an occiput transverse position, with the fetal occiput transverse in the maternal pelvis (Fig 10).
Figure 10 Occiput transverse positions


· With descent, the fetal head rotates so that the fetal occiput is anterior in the maternal pelvis (Fig S-11). Failure of an occiput transverse position to rotate to an occiput anterior position should be managed as an occiput posterior position.
Figure 11. Occiput anterior positions



· An additional feature of a normal presentation is a well-flexed vertex (Fig. 12), with the fetal occiput lower in the vagina than the sinciput.
Figure 12. Well-flexed vertex

· If the fetal head is well-flexed with occiput anterior or occiput transverse (in early labour), proceed with delivery.
· If the fetal head is not occiput anterior, identify and manage the malposition (Table 11).
Diagnosis of malpositions
|
Symptoms and Signs |
Figure |
|
OCCIPUT POSTERIOR POSITION occurs when the fetal occiput is posterior in relation to the maternal pelvis (Fig S-13 and Fig S-14). On abdominal examination, the lower part of the abdomen is flattened, fetal limbs are palpable anteriorly and the fetal heart may be heard in the flank. On vaginal examination, the posterior fontanelle is towards the sacrum and the anterior fontanelle may be easily felt if the head is deflexed. |
FIGURE S-13
FIGURE S-14
|
|
OCCIPUT TRANSVERSE POSITION occurs when the fetal occiput is transverse to the maternal pelvis (Fig S-15). If an occiput transverse position persists into the later part of the first stage of labour, it should be managed as an occiput posterior position. |
FIGURE S-15
|
· If the fetal head is not the presenting part or the fetal head is not well-flexed, identify and manage the malpresentation (Table 12).
OCCIPUT POSTERIOR POSITIONS
Spontaneous rotation to the anterior position occurs in 90% of cases. Arrested labour may occur when the head does not rotate and/or descend. Delivery may be complicated by perineal tears or extension of an episiotomy.
· If there are signs of obstruction or the fetal heart rate is abnormal (less than 100 or more than 180 beats per minute) at any stage, deliver by caesarean section.
· If the membranes are intact, rupture the membranes with an amniotic hook or a Kocher clamp.
· If the cervix is not fully dilated and there are no signs of obstruction, augment labour with oxytocin.
· If the cervix is fully dilated but there is no descent in the expulsive phase, assess for signs of obstruction (Table 10):
- If there are no signs of obstruction, augment labour with oxytocin.
· If the cervix is fully dilated and if:
- the fetal head is more than 3/5 palpable above the symphysis pubis or the leading bony edge of the head is above -2 station, performcaesarean section;
- the fetal head is between 1/5 and 3/5 above the symphysis pubis or the leading bony edge of the head is between 0 station and -2 station:
- Delivery by vacuum extraction and symphysiotomy;
- If the operator is not proficient in symphysiotomy, perform caesarean section;
- the head is not more than 1/5 above the symphysis pubis or the leading bony edge of the fetal head is at 0 station, deliver by vacuum extraction or forceps.
BROW PRESENTATION
In brow presentation, engagement is usually impossible and arrested labour is common. Spontaneous conversion to either vertex presentation or face presentation can rarely occur, particularly when the fetus is small or when there is fetal death with maceration. It is unusual for spontaneous conversion to occur with an average-sized live fetus once the membranes have ruptured.
· If the fetus is alive, deliver by caesarean section.
· If the fetus is dead and:
- the cervix is not fully dilated, deliver by caesarean section;
- the cervix is fully dilated:
- Deliver by craniotomy;
- If the operator is not proficient in craniotomy, deliver by caesarean section.
Do not deliver brow presentation by vacuum extraction, outlet forceps or symphysiotomy.
The chin serves as the reference point in describing the position of the head. It is necessary to distinguish only chin-anterior positions in which the chin is anterior in relation to the maternal pelvis (Fig 24 A) from chin-posterior positions (Fig 24 B).
Figure 24. Face presentation

Prolonged labour is common. Descent and delivery of the head by flexion may occur in the chin-anterior position. In the chin-posterior position, however, the fully extended head is blocked by the sacrum. This prevents descent and labour is arrested.
· If the cervix is fully dilated:
- Allow to proceed with normal childbirth;
- If there is slow progress and no sign of obstruction (Table 10), augment labour with oxytocin;
- If descent is unsatisfactory, deliver by forceps.
· If the cervix is not fully dilated and there are no signs of obstruction, augment labour with oxytocin. Review progress as with vertex presentation.
CHIN-POSTERIOR POSITION
· If the cervix is fully dilated, deliver by caesarean section.
· If the cervix is not fully dilated, monitor descent, rotation and progress. If there are signs of obstruction, deliver by caesarean section.
· If the fetus is dead:
- Deliver by craniotomy;
- If the operator is not proficient in craniotomy, deliver by caesarean section.
Do not perform vacuum extraction for face presentation.
Spontaneous delivery can occur only when the fetus is very small or dead and macerated. Arrested labour occurs in the expulsive stage.
· Replacement of the prolapsed arm is sometimes possible:
- Assist the woman to assume the knee-chest position (Fig 25);
- Push the arm above the pelvic brim and hold it there until a contraction pushes the head into the pelvis.
- Proceed with management for normal childbirth.
Figure 25. Knee-chest position

· If the procedure fails or if the cord prolapses, deliver by caesarean section.
Prolonged labour with breech presentation is an indication for urgent caesarean section. Failure of labour to progress must be considered a sign of possible disproportion (Table S-10)
The frequency of breech presentation is high in preterm labour.
EARLY LABOUR
Ideally, every breech delivery should take place in a hospital with surgical capability.
· Attempt external version if:
- breech presentation is present at or after 37 weeks (before 37 weeks, a successful version is more likely to spontaneously revert back to breech presentation);
- vaginal delivery is possible;
- membranes are intact and amniotic fluid is adequate;
- there are no complications (e.g. fetal growth restriction, uterine bleeding, previous caesarean delivery, fetal abnormalities, twin pregnancy, hypertension, fetal death).
· If external version is successful, proceed with normal childbirth.
· If external version fails, proceed with vaginal breech delivery (see below) or caesarean section.
VAGINAL BREECH DELIVERY
· A vaginal breech delivery by a skilled health care provider is safe and feasible under the following conditions:
- complete (Fig S-20) or frank breech (Fig 21);
- adequate clinical pelvimetry;
- fetus is not too large;
- no previous caesarean section for cephalopelvic disproportion;
- flexed head.
· Examine the woman regularly and record progress on a partograph.
· If the membranes rupture, examine the woman immediately to exclude cord prolapse.
Note: Do not rupture the membranes.
· If the cord prolapses and delivery is not imminent, deliver by caesarean section.
· If there are fetal heart rate abnormalities (less than 100 or more than 180 beats per minute) or prolonged labour, deliver by caesarean section.
Note: Meconium is common with breech labour and is not a sign of fetal distress if the fetal heart rate is normal.
The woman should not push until the cervix is fully dilated. Full dilatation should be confirmed by vaginal examination.
CAESAREAN SECTION FOR BREECH PRESENTATION
· A caesarean section is safer than vaginal breech delivery and recommended in cases of:
- double footling breech;
- small or malformed pelvis;
- very large fetus;
- previous caesarean section for cephalopelvic disproportion;
- hyperextended or deflexed head.
Note: Elective caesarean section does not improve the outcome in preterm breech delivery.
Fetal complications of breech presentation include:
· cord prolapse;
· birth trauma as a result of extended arm or head, incomplete dilatation of the cervix or cephalopelvic disproportion;
· asphyxia from cord prolapse, cord compression, placental detachment or arrested head;
· damage to abdominal organs;
· broken neck.
TRANSVERSE LIE AND SHOULDER PRESENTATION
· If the woman is in early labour and the membranes are intact, attempt external version:
- If external version is successful, proceed with normal childbirth;
- If external version fails or is not advisable, deliver by caesarean section (page P-43).
· Monitor for signs of cord prolapse. If the cord prolapses and delivery is not imminent, deliver by caesarean section.
Note: Ruptured uterus may occur if the woman is left unattended .
In modern practice, persistent transverse lie in labour is delivered by caesarean section whether the fetus is alive or dead.
The transverse lie is the condition when the long axis of the fetus is approximately perpendicular to that of the uterus. When it forms an acute angle, an oblique lie results. An oblique lie is usually only transitory, however, for either a longitudinal or transverse lie commonly results when labor supervenes. For this reason, the oblique lie is termed unstable lie.



Oblique lie


Transverse lie


Persistent transverse lie
An unstable lie is one in which the presenting part alters from week to week. It may be either a transverse or oblique lie or possibly a breech presentation. These are relatively uncommon events but are found in association with the following conditions:
1. Grand multipara. This is by far the commonest factor, due to the lax uterine and abdominal walls, which prevent the splinting effect found in women with lesser parity.
2. Polyhydramnios. The volume of fluid distends the uterus and allows the fetus to swim like a goldfish in a bowl — often taking up an oblique or transverse lie.
3. Prematurity. Here there is a relative excess of fluid to the fetus. If preterm labour occurs, the fetus may be found to have a transverse lie.
4. Subseptate uterus. The septum prevents the fetus from turning in utero.
5. Pelvic tumors such as fibroids and ovarian cysts may not only prevent the lower pole from engaging, but cause it to take up a transverse lie.
6. Placenta praevia. This usually prevents engagement of the presenting part. Because of this it may present with the fetus in an oblique or transverse lie.
7. Multiple pregnancies may present with a transverse lie. If this does occur, it is more common in the second twin.
Diagnosis of the transverse and oblique lies:
1. The external inspection shows than the abdomen is unusually wide from side to side, whereas the fundus of the uterus extends scarcely above the umbilicus.
2. On palpation, with the first maneuver no fetal pole is detected in the fundus.
3. On the second maneuver, a ballottable head is found in one side of uterus and the breech in other.
4. The third and fourth maneuvers are negative unless labor is well advanced and the shoulder has become impacted in the pelvis.
5. When the fetal head is situated in the left side of the uterus the first position of the fetus is identified. When the fetal head is situated in the right side of the uterus the second position is recognized.
6. On vaginal examination, in the early stages of labor, the side of the thorax, if it can be reached, may be recognized above the pelvic inlet. When the dilatation is further advanced, the scapula and the clavicle are distinguished on opposite sides of the thorax. Later in the labor, the shoulder becomes tightly wedged in the pelvic canal, and a hand and arm frequently prolapse into the vagina and through the vulva.
Management of transverse and oblique lie. It is not uncommon for the fetus to have a transverse lie until about the 32nd week of pregnancy. If the transverse lie persists after this time a cause should be determined. An ultrasound examination should be done to exclude placenta praevia, ovarian tumor or fibroid and if either of these conditions are present an elective cesarean section should be performed at 38-39 weeks of gestation. The ultrasound is also used for identifying twins and a subseptate uterus, whilst a vaginal examination will confirm a pelvic tumor.
The main risk of a transverse or oblique lie is in association with preterm rupture of the membranes and cord prolapse. When diagnosed the state of the cervix should be checked. If the cervix is dilated, the patient should be admitted to hospital. If, however, the cervix is closed and the membranes are intact the patient may be reviewed on a regular basis. If no easily identifiable cause is found, attempted external cephalic version can be made after 34 weeks. In grand multipara patients, the fetus will usually turn easily but will often swing back to an abnormal lie. If the abnormal lie persists or constantly reoccurs, the woman should be admitted to hospital by the 38th week. If external version is successful at this stage and the patient's cervix is favorable then artificial rupture of the membrane can be performed with the head held over the pelvic brim and an oxytocin drip commenced to augment uterine activity. If the cephalic presentation is maintained, labor may be allowed to continue.
Management of transverse or oblique in labor - cesarean section must be performed.
Complications of a transverse lie. If a mother goes into labor with a transverse or oblique lie, several catastrophes may occur. Because this occurs more commonly in multiparous women and their uterine activity is often much stronger, rupture of the uterus is more likely. When the membranes rupture there is a greatly increased danger of cord prolapse, prolapse of the arm- persistent transverse lie occur. If the fetus is alive – cesarean section immediately, if die – fetal destroying operation.
DEFLEXED PRESENTATIONS

Fig. 8 Longitudinal lie. Cephalic presentation. Differences in attitude of fetal body in (A) vertex, (B) sinciput, (C) brow, and (D) face presentations. Note changes in fetal attitude in relation to fetal vertex as the fetal head becomes less flexed.
The deflexed vertex presentation. The deflexed vertex presentation is a I degree of head extension.
Diagnosis. The diagnosis of the deflexed vertex presentation bases on the results of the vaginal palpation: the sagittal suture, the large and the small fontanels on the same level. The fetal head presents with a fronto-occipital diameter, a leader point is the large fontanel.
The cardinal movements of labor in deflexed vertex presentation are:
· deflexion;
· internal rotation;
· flexion;
· extension;
· internal rotation of the fetal body and external rotation of the fetal head.
1. Deflexion. The sagittal suture is in the transverse or oblique size of the pelvic inlet. The head fixes to the inlet and some deflexed. The large fontanel becomes the leader point.
2. Internal rotation. This movement is a manner that the occiput gradually moves from its original position posteriorly towards the sacrum os. The rotation is complete when the head reaches the pelvic floor; the sagittal suture is in the anteroposterior diameter.
3. Flexion of the head. Flexion begins when the head fixes by its root of the nose (the first fixing point) to the inferior margin of symphysis pubis. The flexion finishes when the occiput comes to the tip of sacrum and the second fixing point forms.
4. Extension of the head. After internal rotation and flexion the fetal head closely touched with the area of the occiput to the tip of the sacrum. The head extends and deliveries.
5. Internal rotation of the fetal trunk and external rotation of the fetal head. This moment realizes as in anterior occiput presentation.
The brow presentation is a II degree of extension.
With the brow presentation, that portion of the fetal head between the orbital ridge and the frontal suture presents at the pelvic inlet. The fetal head thus occupies a position midway between full flexion (occiput) and full extension (mentum or face). Except when the fetal head is very small or the pelvis is unusually large, engagement of the fetal head and subsequent delivery cannot take place as long as the brow presentation persists.
Diagnosis. The diagnosis of the brow presentation bases on the results of the external obstetrics examination and vaginal palpation. The brow presentation may be recognized by abdominal palpation when both the occiput and chin can be easily palpated. The reliable information can be felt by the vaginal examination: the frontal suture, the large fontanel, orbital ridges, eyes, and root of the nose. The nose and mouth can not be palpable.
The fetal head presents with a mento-occipital diameter, a leader point is the middle of the frontal suture.

Fig.9 Brow posterior presentation.
The delivery at term in brow presentation is impossible. The preterm delivery, when the fetus is small is possible and the characteristically deforms of the head occurred. The caput succedaneum is over the fore head and may be so extensive that identification of the brow by palpation is impossible.
If the labor is possible the cardinal movements in brow presentation are:
1. Deflexion. The frontal suture is in the transverse size of the pelvic inlet. The head fixes to the inlet and deflexed. The middle of the frontal suture becomes the leading point.
2. Internal rotation.
3. Flexion of the head.
4. Extension of the head.
5. Internal rotation of the fetal trunk and external rotation of the fetal head.
Face presentation.
In the face presentation, the head is hyperextended so that the occiput is in contact with the fetal back and the chin (mentum) is presenting part.
Diagnosis. By abdominal palpation the occiput, the chin and the angle between the fetal back and the occiput can be easily palpated. The fetal heart sound are the loudest from the side of the fetal thorax. On vaginal palpation, the distinctive features of the face presentation are the mouth, nose, the malar bones, and the orbital ridges.
Face presentation is rarely observed above the pelvic inlet. The brow generally presents and is converted to a face presentation after further extension of the head during descent through the pelvis.
The cardinal movements of labor in face posterior presentation are:
1. Deflexion. The face linea is in the transverse size of the pelvic inlet. Descent is brought about by the same factors as vertex presentation. The head presented its vertical diameter. The chin is the leading point.
2. Internal rotation. The object of internal rotation of the face is to bring the chin under the symphysis. Only in this way the neck subtend the posterior surface of the symphysis pubis. If the chin rotates directly posteriorly, the birth of the head is impossible.
3. Extension of the head. After the rotation and descent, the chin and mouth appear at the vulva, the undersurface of the chin presses against the symphysis, and the head is delivered by flexion. The nose, eyes, brow and occiput then appeared in succession over the anterior margin of the perineum.
4. Internal rotation of the fetal trunk and external rotation of the fetal head. The shoulders are born as in vertex presentations.

Fig. 10 Biomechanism of labor in face posterior presentation
In the vast majority of deliveries near term the fetus presents by the head, with the best fit into the lower pelvis in the occipito-anterior position. However, although the head is presenting, it may be not in an occipito-anterior but in an occipito-posterior or transverse position. In a few cases the head is grossly deflexed so that the brow or even the face can present.
In other instances, it is not the head that is at the lower pole of the uterus but the buttocks, or breech (from the old English brec—breeches or buttocks). The fetus many even lie transversely so that no pole is in relation to the pelvic inlet. A fetus in this position is undeliverable vaginally; both transverse lies and breech presentations are much more common if the woman enters labour in the earlier weeks of pregnancy (22-28 weeks of gestation).
All these malpresentations and malpositions need careful diagnosis and skilful management.
Malpositions
Normal mechanism
Usually the fetal head engages in the left (less commonly, right) occipito-anterior position and then undergoes a short rotation to be directly occipito-anterior in the mid-cavity.
Occipito-posterior position
This is the commonest malpresentation. The head engages in the left or right occipito-transverse position, and the occiput rotates posteriorly, rather than into the more favourable occipito-anterior position. The reasons for the malrotation are often unclear. A flat sacrum or a head that is poorly flexed may be responsible; alternatively, poor uterine contractions may not push the head down into the pelvis strongly enough to produce correct rotation; epidural analgesia might sometimes relax the pelvic floor to an extent that the fetal occiput sinks into it rather than being pushed to rotate in an anterior direction. The diagnosis is determined clinically by vaginal examination.
The best management is to await events, preparing the woman and staff for a long labour. Progress should be monitored by abdominal and vaginal assessment, and the mother’s condition should be watched closely. Good pain relief with an epidural and adequate hydration are required.
The mother may have an urge to push before full dilation, but the midwife should discourage this. If the occiput comes directly into the posterior position (face to pubis) a vaginal delivery is possible if the pelvic diameters are reasonable.
Figure If, instead of the normal curve, the sacrum is straightened (shaded area), the anterior-posterior diameter in mid-cavity is reduced (A-A), thus hindering head rotation in this zone
Occipito-transverse position
The head engages in the left or right occipito-transverse position, but then rotation to occipito-anterior fails to occur and the head remains in the transverse position. If the second stage is reached the head must be manually rotated, rotated with appropriate forceps (namely, those with no pelvic curve—for example, Kielland’s forceps), or delivered using vacuum extraction.
Such vaginal deliveries must not be undertaken if there is any acidosis (fetal blood pH <7.15) as cerebral haemorrhage may result. They are now often undertaken in the operating theatre (trial of forceps) so that a rapid change to caesarean section can be made if there is any difficulty. Some obstetricians have abandoned these more difficult vaginal deliveries in favour of caesarean section.
Figure Three methods of delivering a baby in occipito-transverse position in the second stage of labour: (a) vacuum extraction with a linear pull, so allowing rotation to occur according to the pelvic anatomy; (b)rotation and extraction with Kielland’s ...
Face and brow positions
If there is a complete extension of the fetal head, the face will present for delivery. Labour will be longer, but if the pelvis is adequate and the head rotates to a mentoanterior position, a vaginal delivery can be expected. If the head rotates backwards to a mentoposterior position a caesarean section is needed.
In a brow presentation the fetal head stays between full extension and full flexion so that the biggest diameter (the mento-vertex 13 cm) presents. This is usually only diagnosed once labour is well established. Unless the head flexes, a vaginal delivery is not possible, and a caesarean section is required.
Figure Left: Abdominal features of a face presentation; the head is felt on the same side as the back and is often not engaged. Right: Abdominal features of a brow presentation—both the sinciput and the occiput are equally palpable on each side of the ...
Malpresentations
Breech
This is the commonest malpresentation. It is usually discovered before labour, although one third are not diagnosed until during labour, when vaginal examinations allow a more precise diagnosis to be made, especially as the cervix dilates and allows direct palpation of the presenting part of the fetus. Current opinion holds that in late pregnancy, external cephalic version should be offered, with the use of tocolytics in nulliparous women to relax the uterus. This procedure is successful in 40% of nulliparous women, and 60% of multiparous women if performed after 38 weeks. If breech presentation persists, preparations for delivery are made. Delivery should be in a hospital with an experienced midwife and obstetrician actively involved. An anaesthetist and paediatrician should be available.
All women with malpresentations and malpositions should be delivered in hospital
Vaginal delivery of breech presentation
· The mother should be in the lithotomy position (laterally tilted to avoid supine hypotension)
· The bladder should be emptied
· An anaesthetist and a paediatrician should be present
· An episiotomy is advisable
· The breech, legs, and abdomen should be allowed to deliver spontaneously (the legs can be assisted by flexing)
· The shoulders can be encouraged to deliver by rotation of the trunk (Lövsett’s manoeuvre)
· Delivery of the head should be controlled manually or with forceps
With a normal pelvis and the fetus’s weight estimated by ultrasonography to be 2500-4000 g, assisted breech delivery in experienced hands is probably as safe as a caesarean section. These days many women with a breech presentation choose to have a caesarean section as they think this is the safest method of delivery. In the past doctors have led them to believe this, but meta-analyses of randomised controlled trials do not substantiate this view. Of those women who aim for a vaginal delivery, about half will succeed. Before 32 weeks, caesarean section is commonly performed for a breech presentation, although the evidence of its effectiveness even at this gestation is not strong; the operation can be technically difficult, leading to maternal complications (see next article).
Breech delivery is an art that all those practising obstetrics need to learn, with supervision by senior practitioners, because unexpected breech deliveries still occur.
Transverse lie
When the fetus is lying sideways with the head in one flank and the buttocks in the other, it cannot be born vaginally. Unless it converts or is converted in late pregnancy, a caesarean section is required. After opening the abdominal wall, the surgeon may be able through the wall of the uterus to rotate the fetus so that it then becomes a longitudinal lie. If not, the uterine incision must be so placed transversely to allow access to a fetal pole.
Nowadays internal podalic version is not often attempted in transverse lies; a caesarean section is thought to be safer, although it can be a difficult operation
Figure Transverse lie with subseptate uterus and low lying placenta
Prolapsed umbilical cord
If the presenting part of the fetus does not fit the pelvis after membrane rupture, the umbilical cord can slip past and present at the cervix, or actually prolapse into the vagina. If such an event is diagnosed in labour, the woman should be transferred straight to a hospital, preferably in a steep lateral or knee chest position with a midwife holding up the presenting part with fingers in the vagina, to stop it compressing the umbilical cord during contractions. A caesarean section is needed urgently.
If the cord is found ahead of the presenting part before membrane rupture, the membranes should be ruptured artificially only if full preparations for an emergency caesarean section have been made. The cord often slips to one side of the head and disappears when the membranes rupture.

A prolapsed umbilical cord is common in breech deliveries. This happens when part of the umbilical cord slips down through the cervix before the baby does. The cord is then compressed during contractions, which cuts down on blood flow to the baby. An emergency cesarean section is usually needed.
Figure Prolapsed cord into the vagina after membrane rupture with a high head
Shoulder dystocia
After delivery of the head the hardest part of delivery is usually over, but occasionally the shoulders are slightly broader than usual, with a bisacromial diameter greater than 10 cm. The shoulders usually adopt the antero-posterior axis to negotiate the outlet. If the shoulders are still above the brim at this stage, no advance occurs. The baby’s chest is trapped within a vaginal cuirass. Although the nose and mouth are outside, the chest cannot expand with respiration. There is currently no way of predicting this problem reliably. The fifth annual report from the confidential inquiry into stillbirths and deaths in infancy (1998) considers the problem well.
Shoulder dystocia: best delivery method
· Flex and abduct the mother’s thighs as much as possible (the McRoberts procedure) and then depress the baby’s head towards the mother’s anus, with an assistant applying suprapubic pressure
· If this does not work, then manual rotation of the baby through 180° by vaginal and abdominal pressure may succeed
· Cleidotomy or symphysiotomy is the last resort and should be attempted only by an experienced obstetrician
Multiple pregnancies
Multiple pregnancies are increasing in frequency in Britain, mainly as a result of infertility treatment (both ovarian stimulation and in vitro fertilisation). Nearly all multiple pregnancies are now diagnosed early by ultrasound examination. Some twins, however, die and are absorbed in the first half of pregnancy (the disappearing twin syndrome). When pregnant with twins, most women go into labour early at about 37 weeks. The woman should be in labour in a hospital with a special care baby unit. With no complicating factors, the mother can go into spontaneous labour provided that the first twin is lying longitudinally. It is wise to have an intravenous line running. Labour usually proceeds rapidly; although each fetus is small, the total content of the uterus is large. The fetal heart rates of each twin should be monitored separately; some cardiotocographs allow this to be shown on a single chart. An anaesthetist should be present at delivery, and an epidural makes delivery of the second twin easier if there is a malpresentation (which occurs in 5-15% of cases). Paediatricians also should be present at the second stage of labour.
Multiple births in United Kingdom, 1995
|
Type of multiple birth |
No of multiple births (rate per 1000 maternities*) |
Ratio of multiple to singleton births |
|
Twins |
|
1:73 |
|
Triplets |
|
1:2282 |
|
Quadruplets |
|
1:72 563 |
|
Total |
10 217 (14.0) |
1:71 |
Data supplied by Multiple Births Foundation.
*A maternity is any pregnancy that results in the birth of at least one live baby; the total number of maternities in 1995 was 725 638.
Conclusions
· Women with a fetus with an abnormal presentation or position should be transferred to hospital for the best care
· Problem cases should be anticipated
· Emergencies during an apparently normal labour need the immediate attention of a skilled obstetrician
· Prepared protocols ensure that all members of the labour ward team know their function and what should be done
After the first twin is delivered, the cord should be clamped and the lie of the second twin assessed carefully. This can be done clinically, but ultrasound scanning is more reliable. If the lie is not longitudinal, it should be made so by an external cephalic or internal podalic version. Unless uterine contractions return within 15 minutes, stimulation of the uterus with dilute oxytocin should be started, with an aim of delivering the second twin 25-45 minutes after the first. If there is any difficulty in delivery of the second twin, or if this twin develops a bradycardia, a vacuum extraction (in a cephalic presentation) or a breech extraction, if the fetus is lying the other way, can be performed. Internal podalic version and breech extraction is usually easy in this situation. It is not necessary to resort automatically to a caesarean section.





























