The musculoskeletal system provides shape and support to the body, allows movement, protects the internal organs, produces red blood cells in the bone marrow (hematopoiesis), and stores calcium and phosphorus in the bones. Although examining this system is usually only a small part of the overall physical assessment, everything we do depends on an intact musculoskeletal system. How extensive an assessment you perform depends largely on each patient’s problems and needs.
Perform a comprehensive musculoskeletal assessment if you detect a musculoskeletal abnormality or uncover a symptom that suggests musculoskeletal involvement. Musculoskeletal problems are common in all age groups. Primary problems may result from congenital, developmental, infectious, neoplastic, traumatic, or degenerative disorders of the system itself. Secondary problems can result from disorders of other body systems.
The goal of a complete musculoskeletal assessment is to detect risk factors, potential problems, or musculoskeletal dysfunction early and then to plan appropriate interventions, including teaching health promotion and disease prevention and implementing treatment measures. By doing so, you can play a significant role in preventing pain and dysfunction in your patients.
Performing the Musculoskeletal Assessment
Health History. Obtaining a thorough and accurate health history is crucial to your assessment of the musculoskeletal system. As the health history interview progresses, clarify exactly what the patient means by certain subjective complaints, including the location, character, and onset of any symptoms. Only the patient can give you data regarding pain, stiffness, ability to move,and how daily activities have been affected.
The history provides the subjective data that will direct the physical examination. If time is an issue and you are unable to perform a complete health history, perform a focused history on the motor-musculoskeletal system.

Biographical Data. A review of the biographical data may identify patients who are at risk for musculoskeletal problems. Consider the patient’s age, sex, marital status, race, ethnic origin, and occupation as possible risk factors. For example, women are at a higher risk than men for osteoporosis and rheumatoid arthritis (RA); an occupation that requires heavy lifting increases the risk for injury to muscles, joints, and supporting structures; and the risk for degenerative joint disease (DJD; osteoarthritis) increases with age. Even a patient’s address may have significance. For example, Lyme disease,which has musculoskeletal repercussions, is endemic on the northeast coast from Massachusetts to Maryland, in the midwest states of Wisconsin and Minnesota, and on the west coast from northern California to Oregon.
Current Health Status. Begin your assessment with questions about the patient’s current health status, because she or he is most interested in this.The major symptoms to watch for, in order of importance, are pain,weakness, and stiffness.
Symptom Analysis.
Pain. Pain can result from bone, muscle, or joint problems. Bone pain is not usually associated with movement unless there is a fracture, but muscle pain is. Current or recent illness can cause muscle aches.Bone pain is deep, dull, and throbbing;muscle pain takes the form of cramping or soreness. In RA, joint pain and stiffness are worse in the morning. In osteoarthritis, the joints are stiff after rest and pain is worse at the end of the day.
Weakness. Muscle weakness associated with certain diseases migrates from muscle to muscle or to groups of muscles. Knowing the symptom patterns and when they occur can help identify the disease process responsible for weakness. Identifying the weakness related to proximal or distal muscle groups is also helpful.Proximal weakness is usually a myopathy;distal weakness is usually a neuropathy.
Be sure to ask the patient if the weakness interferes with his or her ability to perform everyday activities. For example, proximal weakness of the upper extremities often presents itself as difficulty lifting objects or combing hair. Proximal weakness of the lower extremities presents as difficulty with walking and crossing the knees. Patients with polymyalgia rheumatica have proximal muscle weakness. A distal weakness of the upper extremities is manifested by difficulty in dressing or turning a doorknob. Patients with myasthenia gravis have difficulty with diplopia, swallowing, and chewing, along with generalized muscle weakness.
Stiffness. Stiffness is a common musculoskeletal complaint. It is important to ascertain if the stiffness is worse at any particular time of the day. For example, patients with RA are stiff on arising because of the period of joint rest that occurs during sleep.
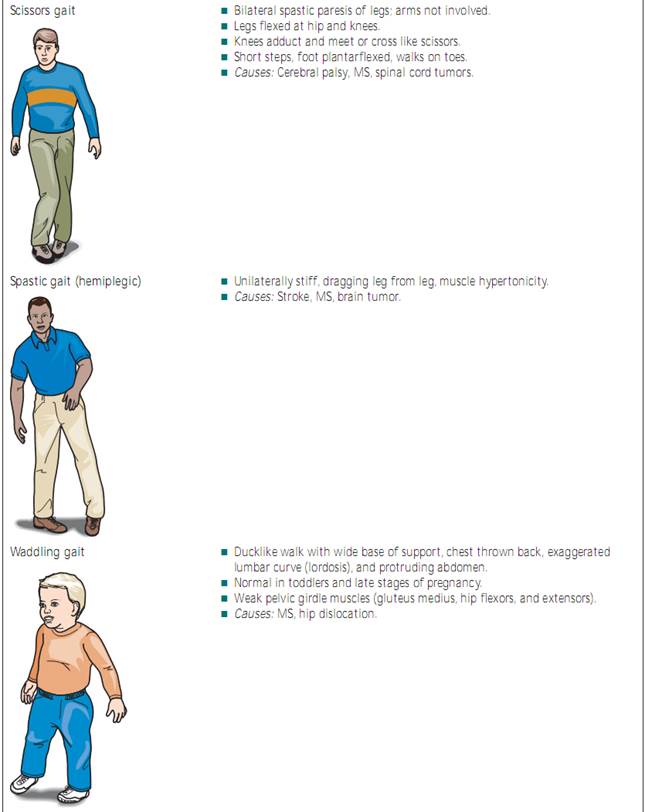
Balance and Coordination Problems. Problems with balance and coordination often indicate a neurological problem. These problems often manifest as gait problems or difficulty in performing activities of daily living (ADLs). The patient may complain of falling or losing balance or may have ataxia—irregular and uncoordinated voluntary movements.Gait problems are associated with cerebellar disorders, Parkinson’s disease, multiple sclerosis (MS),herniated disc, stroke,Huntington’s chorea, brain tumor, inner ear problems, medications, and exposure to chemical toxins.
Other Related Symptoms. Certain musculoskeletal diseases may produce multiple symptoms. For example, acute rheumatic fever, gout, and autoimmune inflammatory diseases may cause fever and joint pain. A woman with back pain and vaginal discharge may have a gynecological disease. Lower back pain and weight loss suggest tuberculosis (TB) of the spine.Bowel and bladder dysfunction suggest a herniated disc.Therefore, also ask the patient:“Do you have a sore throat, fever, joint pain, rash,weight loss, diarrhea, numbness, tingling, or swelling?”
Past Health History. After taking the past health history, compare it with the patient’s present musculoskeletal status or uncover risk factors that might predispose the patient to musculoskeletal disorders.

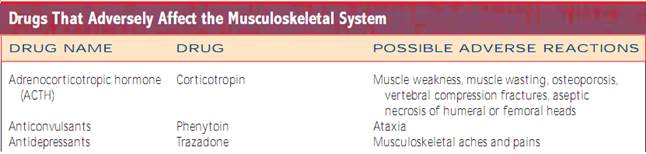
Family History. The purpose of the family history is to identify predisposing or causative factors for musculoskeletal problems.After assessing the current and past musculoskeletal health status, investigate possible familial tendencies toward problems.

Review of Systems. The review of systems (ROS) allows you to assess the interrelationship of the musculoskeletal system to every other system. Often, you may uncover important facts that your patient failed to mention earlier.

Psychosocial Profile. The psychosocial profile can reveal patterns in the patient’s life that may affect the musculoskeletal system and put her or him at risk for musculoskeletal disorders.

Physical Assessment. Now that you have collected the subjective data, begin collecting the objective data by means of the physical examination. Keep all pertinent history findings in mind as you proceed. These findings, along with those from the physical examination, will complete the assessment picture.Then you can analyze the data, formulate nursing diagnoses, and develop a plan of a care. Because a musculoskeletal problem might be present, you will need to know normal musculoskeletal function before you can determine abnormal findings. The anatomy will direct your assessment.
Approach. Physical assessment of the musculoskeletal system provides data on the patient’s posture, gait, cerebellar function and bone structure,muscle strength, joint mobility, and ability to perform ADLs. You will use inspection, palpation, and percussion to assess the musculoskeletal system. Be systematic in your approach, working from head to toe and comparing one side with the other. Inspect and palpate each joint and muscle; then assess range of motion (ROM) and test muscle strength. Perform inspection and palpation simultaneously during this assessment.
Performing a General Survey. Before examining specific areas, scan the patient from head to toe, looking for general appearance and signs of musculoskeletal problems. For example:
- Obtain the patient’s vital signs. Elevations in temperature are associated with Lyme disease, RA, and infections such as osteomyelitis.
- Be alert for signs of pain or discomfort as your patient performs ROM. If signs or symptoms of pain are present with movement, never force a joint.
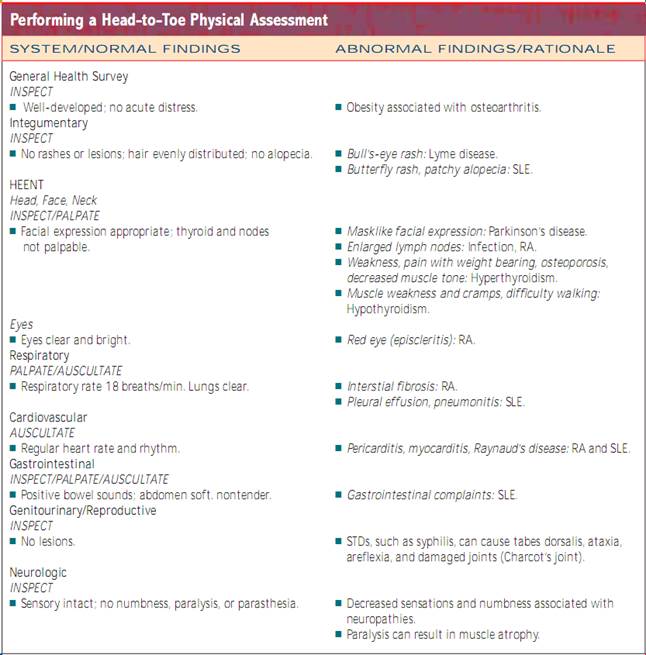
Performing a Head-to-Toe Physical Assessment. Now look for changes in every system that might signal a musculoskeletal problem.
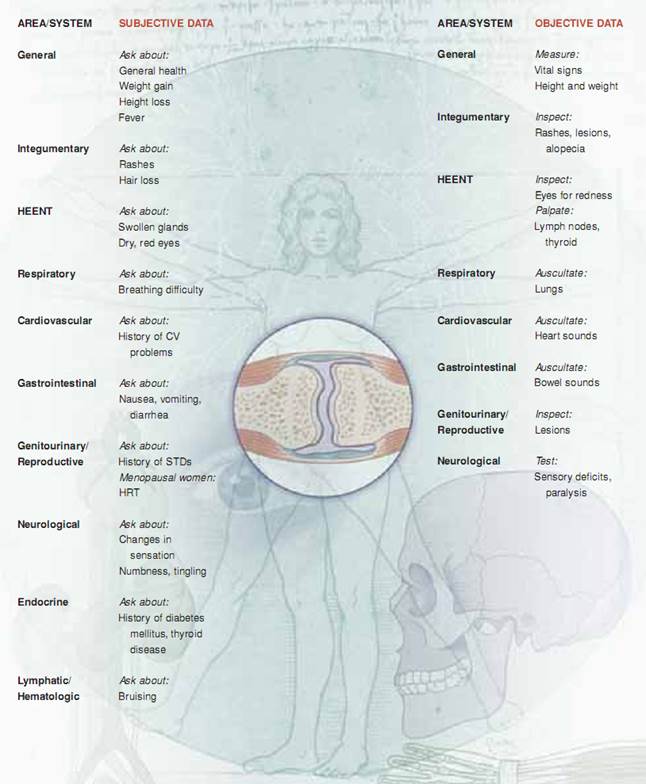

Performing a Musculoskeletal Physical Assessment. Now that you have completed a head-to-toe scan, focus on the specifics of the examination. Proceed in this order:
- Assess posture, gait, and cerebellar function.
- Measure limbs.
- Assess joints and test joint movement.
- Assess muscle strength and ROM.
- Perform additional tests to assess for wrist, spine, hip, and knee problems, if necessary.
Assessing Posture, Gait, and Cerebellar Function.
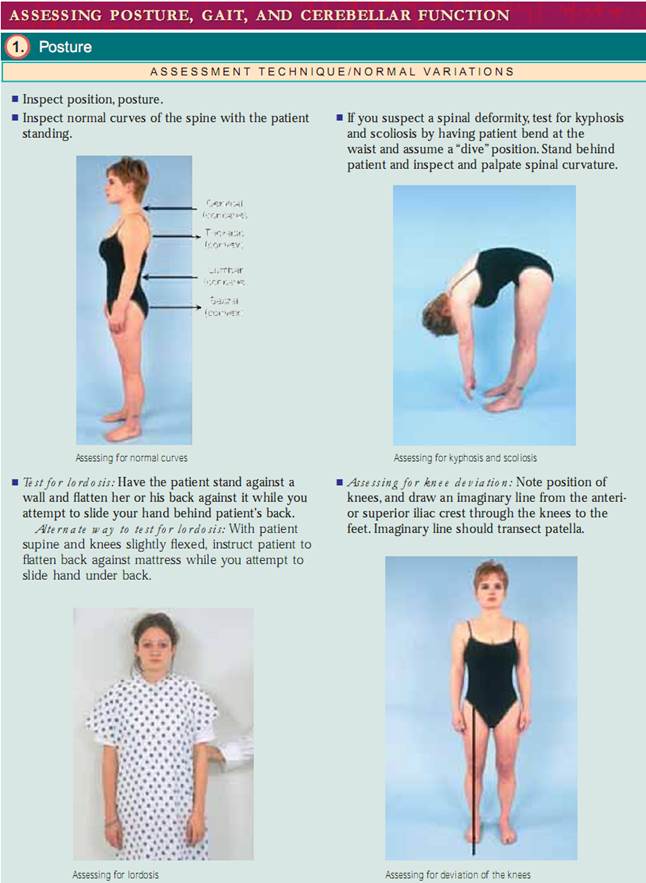
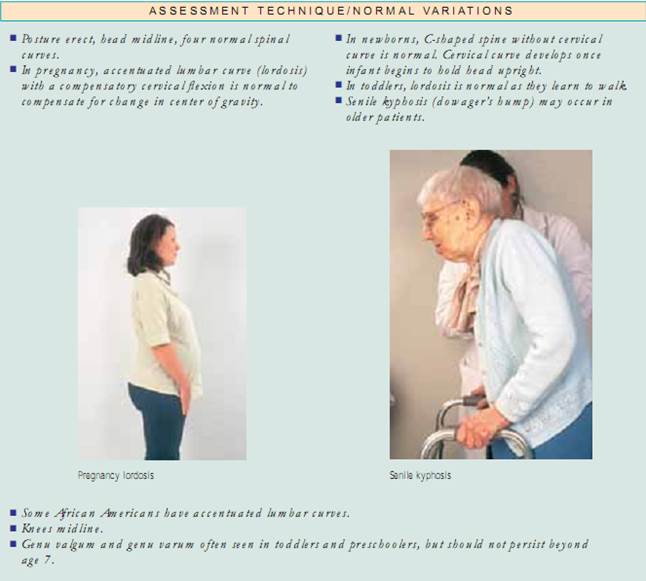
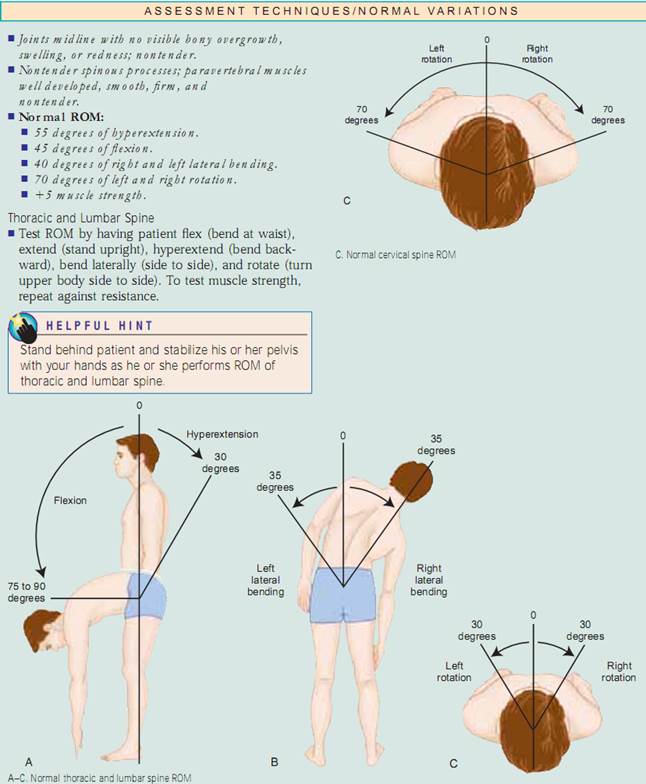
Posture. Begin by assessing your patient’s posture, or his or her position in relation to the external environment. Posture should be erect,with the head midline.The spine is best assessed with the patient standing. Inspect from the front, back, and side, looking for alignment and noting symmetry of shoulders, scapula, and iliac crests. Adults have four normal curvatures. The cervical and lumbar curves are concave, and the thoracic and sacral curves are convex.When assessing for spinal curvature deformities, it is important to determine if the deformity is structural or functional (postural) in nature. To assess for kyphosis and scoliosis, have the patient bend forward from the waist with her or his arms relaxed and dangling.Then stand behind the patient to check for curvatures.The curvatures disappear in functional kyphosis and scoliosis but remain in the structural form. To assess for lordosis,have the patient stand against a wall and flatten her or his back against it. If you can freely slide your hand through the lumbar curve, the patient has structural lordosis. An alternative method is to have the patient lie supine with the knees slightly flexed and attempt to flatten her or his lumbar curve. If she or he can, the lordosis is functional. Next, have your patient stand erect with the feet together and note the position of the knees. Are the knees midline? Draw an imaginary line from the anterior superior iliac crest to the feet. Normally, this line should transect the patella. Note if the patella deviates away from the midline.Normally, the knees should be less than 2.5 cm (1") apart and the medial malleoli (ankle bones) less than 3 cm (11⁄8") apart.
Gait. Next,assess your patient’s gait.Pay particular attention to the base of support (distance between the feet) and stride length (distance between each step). Is there a wide base of support? The average base of support for an adult is about 2 to 4 inches.The average stride length for an adult is about 12 to 14 inches. Stride length depends in part on leg length, so the longer the legs, the greater the stride length.
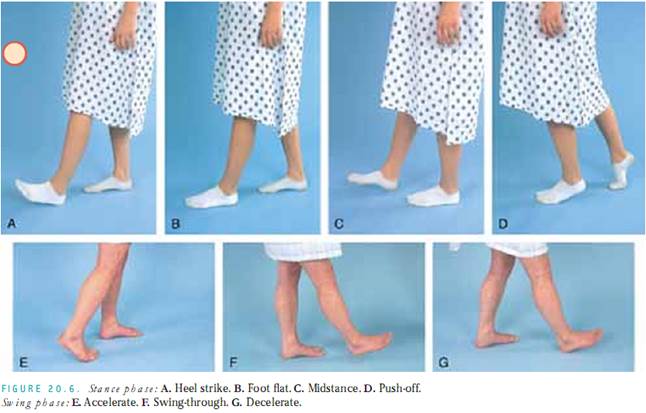
Also pay attention to the phases of the gait—stance and swing. The stance phase has four components: heel strike, foot flat,midstance, and push-off. During midstance, the weight shifts to bearing the full body weight. The swing phase has three components: accelerate, swing-through, and decelerate. Figure 20.6 illustrates the two phases and their components. If you do not detect a gait problem, chart “phases conform.” If you do detect a problem, try to identify the specific portion of the gait that is abnormal.For example, someone with left-sided weakness from a stroke may have problems with the acceleration portion of the swing phase and the midstance portion of the stance phase. Continue to observe your patient’s gait, taking note of posture and cadence as he or she walks.Ask yourself: Do the arms swing in opposition? Is there toeing in or out? Are movements smooth and coordinated?
Cerebellar Function. Now, assess cerebellar function, including balance, coordination, and accuracy of movements.
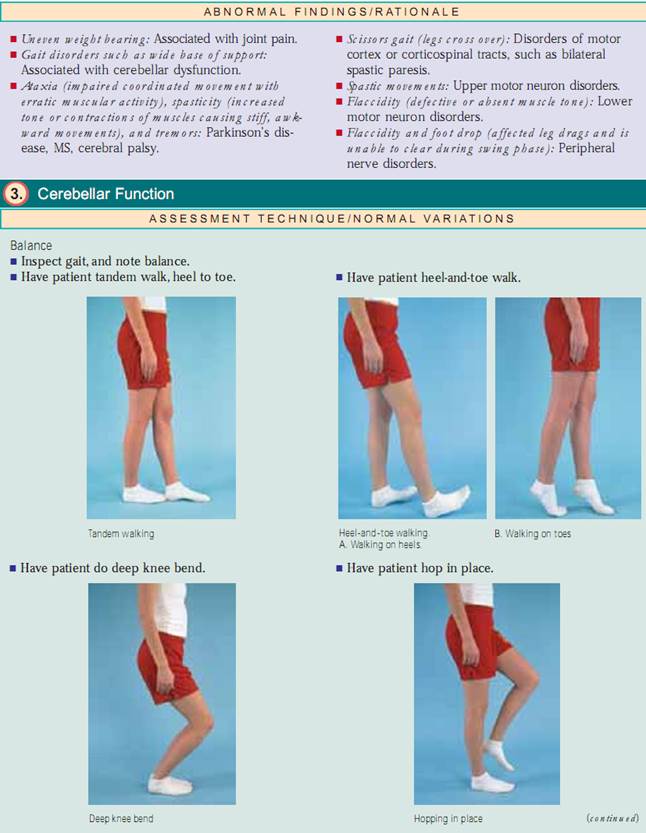
Balance. To assess balance, look at your patient’s gait. If he or she has a gait problem,you will be unable to proceed further. If there are no gait problems, have the patient tandem (heel-to-toe) walk, heel-and-toe walk, hop in place, do a deep knee bend, and perform the Romberg test.To perform the Romberg test, have the patient stand with feet together and eyes open; then have him or her close the eyes. If cerebellar function is intact,he or she will be able to maintain balance with minimal swaying with eyes closed (negative Romberg test). Keep in mind that balance problems may also occur with inner ear disorders.
Coordination. Next, assess coordination. Note the patient’s dominant side.Usually this side is more coordinated.To test upper extremity coordination, have the patient perform rapid alternating movements (RAMs) by patting her or his thigh with one hand, alternating between the supinate and the pronate hand position.Have her or him perform finger-thumb opposition to further test hand coordination. To test lower extremity coordination, have the patient perform rhythmic toe tapping and then run the heel of one foot down the shin of the opposite leg. Remember to test each side separately and compare findings.
Accuracy of Movements. Point-to-point localization is used to assess accuracy of movements. Have the patient touch his or her finger to the nose with the eyes open, then closed.Or have him or her touch your finger at various positions.



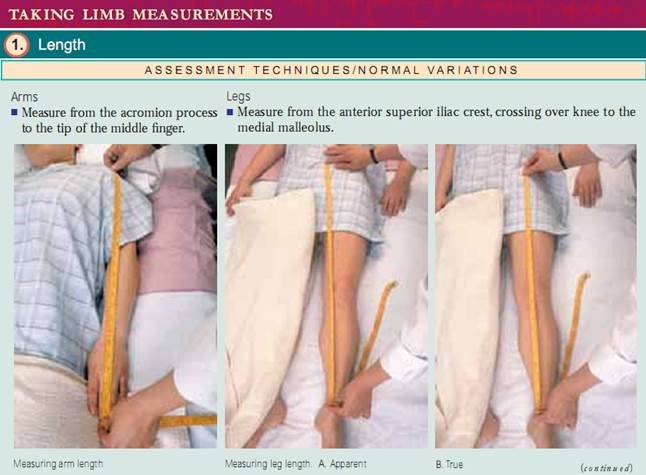
Taking Limb Measurements. Limb measurements include both length and circumference.Measure arm lengths from the acromion process to the tip of the middle finger.Measure leg lengths from the anterior superior iliac crest crossing over the knee to the medial malleolus.This is referred to as true leg length. An apparent leg length measurement is measured from a nonfixed point, the umbilicus, to the medial malleolus.
A true leg length discrepancy results from bone length inequality, whereas an apparent leg length discrepancy may result from a pelvic tilt or flexion deformity of the hip. Discrepancies between right and left should not exceed more than 1 cm. Obviously, a leg length discrepancy usually results in clinical problems such as gait disorders or hip or back pain.
Limb circumference reflects actual muscle size or muscle mass. Measure circumference on forearms, upper arms, thighs,and calves.Take note of the patient’s dominant side,which may normally be up to 1 cm larger than her or his nondominant side. To ensure accurate circumference measurement, determine the midpoint of the extremity being assessed. For example, if you are measuring upper arm circumference, measure the distance from the acromion process to the olecranon process, and use the midpoint to determine circumference; then do the same for the opposite arm.
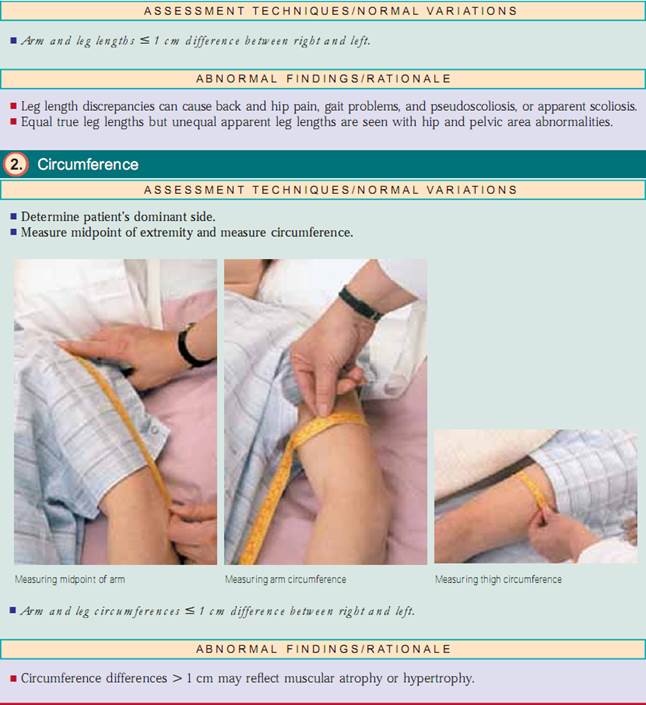
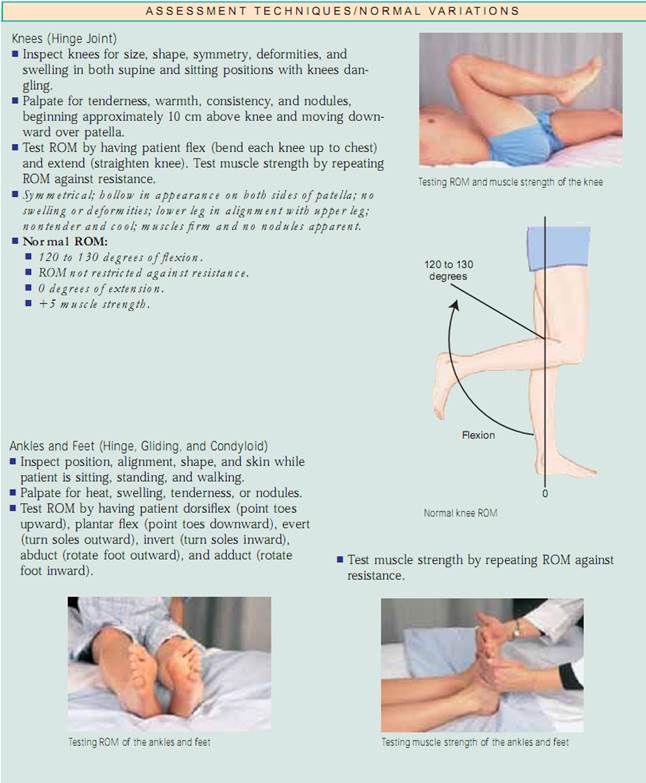
Assessing Joints and Muscles. Inspect the size, shape,color,and symmetry of each joint, noting masses,deformities, and muscle atrophy.Compare muscle and joint findings bilaterally and palpate for edema, heat, tenderness, pain, nodules, crepitus, and stability. Test active ROM (in which the patient performs the movement) and passive ROM (in which you put the joint through the ROM) of the joint (Fig. 20.7). Changes in articular cartilage, scarring of the joint capsule, and muscle contractures all limit motion. It is important to determine the types of motion the patient can no longer perform, especially the ADLs.
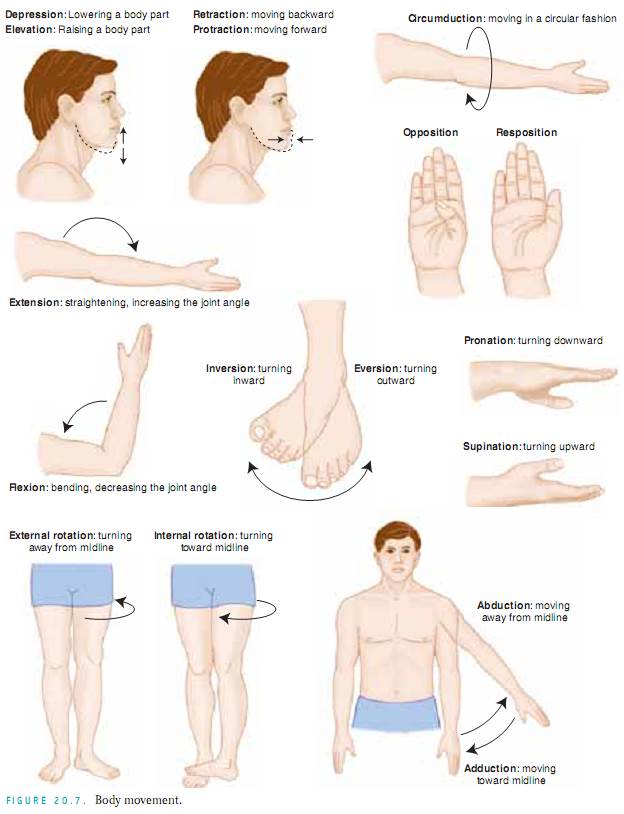
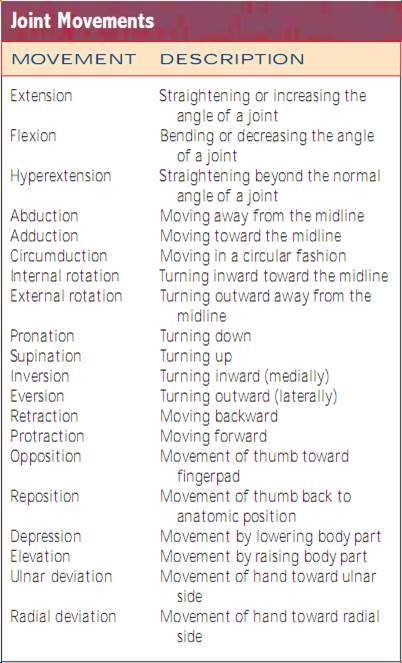
Joint clicking or crepitus may occur normally sometimes or may be associated with dislocations of the humerus, temporomandibular joint (TMJ) problems, displacement of the biceps tendon from its groove, damaged knees, or DJD.
Joint deformity may result from a congenital malformation or a chronic condition. In any patient with a deformity, ask the following questions:
- When did you first notice the deformity?
- Did the deformity occur suddenly?
- Did it occur as the result of trauma?
- Has the deformity changed over time?
- Has it affected your range of motion?
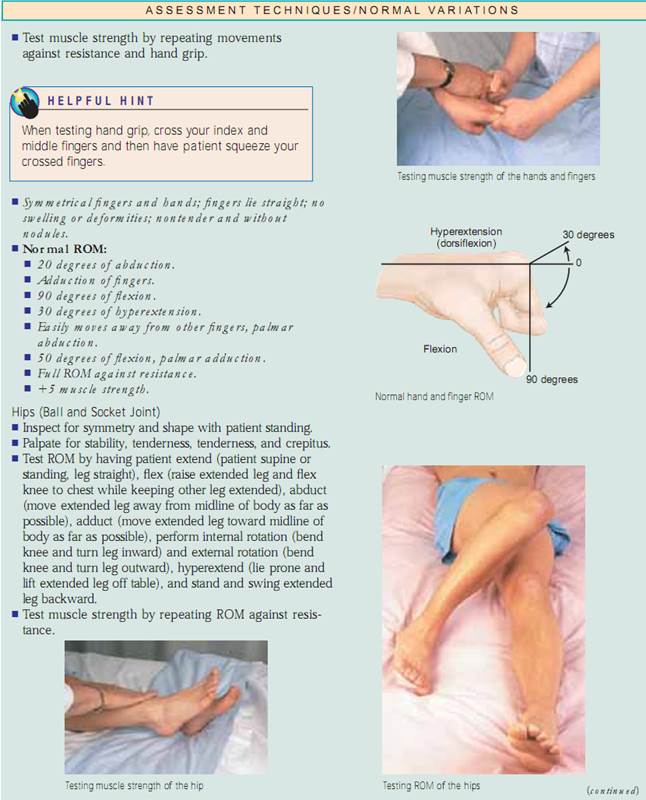
Test muscle strength by asking the patient to put each joint through ROM while you apply resistance to the part being moved.If the patient is unable to move the part against resistance, then ask him or her to perform the ROM against gravity. If this cannot be performed, attempt to passively put the muscle through ROM. If this is not possible (because of a contracture),palpate the muscle while the patient attempts to move it.Document muscle strength as shown in the box entitled Rating Scale for Muscle Strength.

Begin your assessment by inspecting and palpating the muscles of the upper and lower extremities.Assess muscle tone and mass in both relaxed and contracted state, and then assess each joint and test muscle strength as the patient performs ROM.
Additional Tests. You can perform the following additional tests to assess for wrist, spinal, hip, and knee problems.
Tests for Wrist Problems.
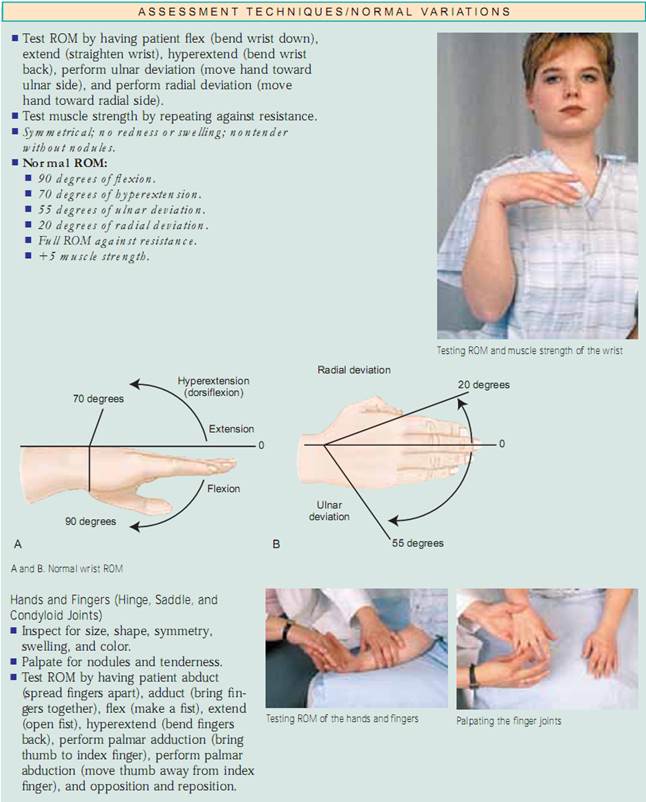
Phalen’s Test. Have the patient flex the hands back to back at a 90-degree angle and hold this position for about 1 minute (Fig.20.8). If the patient complains of numbness or tingling anywhere from the thumb to the ring finger, the test is positive for carpal tunnel syndrome.
Tinel’s Test. Percuss lightly over the median nerve, located on the inner aspect of the wrist (Fig. 20.9). If numbness and tingling occur on the palmar aspect of the wrist and extend from the thumb to the second finger, the test is positive for carpal tunnel syndrome.


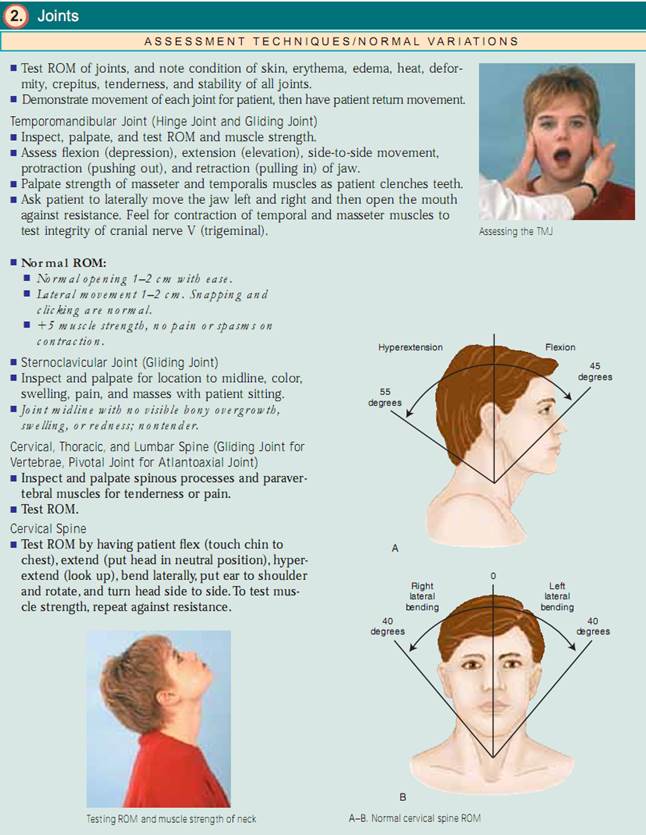

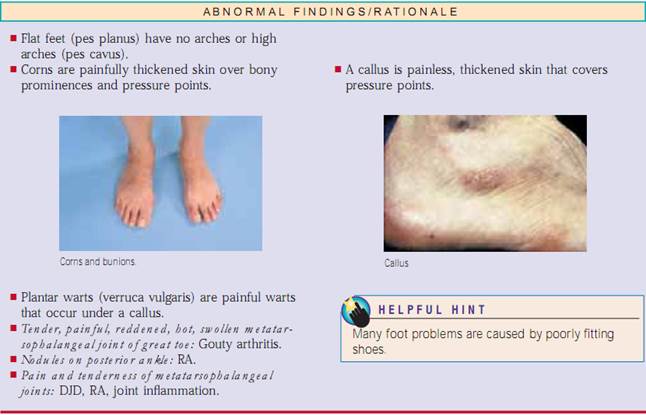
Test for Arm Problems.
Pronator Drift. Perform this test if you detect muscle weakness of the arms. Have the patient stand with arms extended, hands supinated, and eyes open and then closed for at least 20 to 30 seconds (Fig.20.10).Check for downward drift and pronation of the arms and hands. Pronation and drift of one arm is called pronator drift and may indicate a mild hemiparesis. Flexion of the fingers and elbow may accompany pronator drift.A lateral and upward drift may also occur in patients with loss of position sense. If your patient is able to hold her or his arms extended without drift, gently tap downward on the arms. If she or he has normal muscle strength, coordination, and position sense, the arms will return to the horizontal position. A weak arm is easily displaced and does not return to the horizontal position.
You can also assess drifting and weakness by having the patient hold his or her arms over the head for 20 to 30 seconds.Then, try to force the arms down to the sides as the patient resists.Drifting or weakness may indicate a hemiparesis.

Test for Spinal Problems.
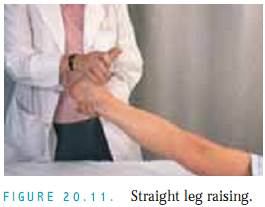
Straight Leg Raising (Lasègue’s Test). Perform this test when the patient complains of low back pain that radiates down the leg (sciatica). This test checks for a herniated nucleus pulposus.Ask the patient to lie flat and raise the affected leg to the point of pain (Fig.20.11).Pain and sciatica that intensify with dorsiflexion of the foot are a positive sign for a herniated disc.
Tests for Hip Problems.
Thomas Test. This test assesses for hip flexure contractures hidden by excessive lumbar lordosis. Have the patient lie supine with both legs extended and then flex one leg to her or his chest (Fig.20.12).The test is positive if the opposite leg raises off the table. Repeat the same maneuver on the opposite side.

Trendelenburg Test. This test is used to assess for a dislocated hip and gluteus medius muscle strength. Have patient stand erect and check the iliac crest—it should be level. Then, have the patient stand on one foot and check again. If the iliac crest remains level or drops on the side opposite the weight-bearing leg, the gluteus medius muscle is weak or the joint is not stable and there may be a hip dislocation on the weightbearing side.
Tests for Knee Problems. Perform one of the following two tests if you noted swelling secondary to fluid accumulation or soft tissue damage.
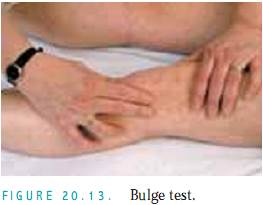
Bulge Test. Perform this test if you suspect small amounts of fluid.With the patient supine, stroke the medial side of the knees upward several times to displace the fluid.Then, press the lateral side of the knee, and inspect for the appearance of a bulge on the medial side (Fig.20.13).
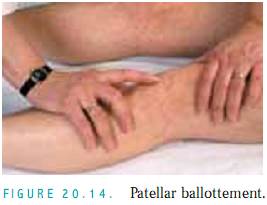
Patellar Ballottement. Perform this test if you suspect large amounts of fluid. With the patient supine, press firmly with your left thumb and index finger on each side of the patella (Fig. 20.14). This displaces fluid into the suprapatellar bursa between the femur and the patella. Then, gently tap on the kneecap. If fluid is present, the patella will bounce back to your finger (floating kneecap).
Lachman Test. If your patient complains that his or her knee gives way or buckles, test anterior,posterior,medial, and lateral stability. To test medial and lateral stability, have the patient extend the knee and attempt to abduct and adduct it.Normally,no movement should occur if the knee is stable. To assess the anterior and posterior plane, have the patient flex the knee at least 30 degrees. Stabilize and grasp the leg below the patella, and attempt to move it forward and back. If the joint is stable, no movement should occur (Fig. 20.15).Another similar test for stability of the anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL) is the drawer test.With the patient’s knee flexed at a 90-degree angle, apply anterior and posterior pressure against the tibia, and feel for movement.Movement of the tibia is a positive draw sign, indicating an ACL or PCL tear.

To test stability of the collateral ligament, have the patient lie supine with the knee slightly flexed.Place your hand at the head of the fibula and apply pressure medially; then reverse and apply pressure laterally. If the joint is unstable, movement will occur and create a palpable medial or lateral gap at the joint.
Perform one of the following tests if your patient complains of clicks or knee-locking and you suspect a torn meniscus.
McMurray’s Test. To perform McMurray’s test, position the patient supine with her or his knee fully flexed (Fig. 20.16). Place one hand on the heel and the other on the knee and gently internally and externally rotate the foot as you bring the leg to full extension.The test is positive if audible or palpable clicks occur or the knee locks.

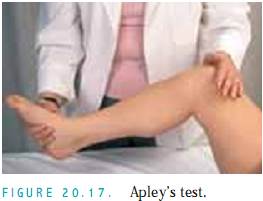
Apley’s Test. Position the patient supine with his or her knee flexed at 90 degrees (Fig. 20.17).Place one hand on the heel and the other hand on the knee.Apply pressure with both hands and gently rotate the foot. The test is positive if audible or palpable clicks occur.

SUMMARY
- This chapter taught you how to do a thorough musculoskeletal assessment, including a health history and physical examination.
- Before you begin the assessment, you need an understanding of the anatomy of the musculoskeletal system including ROMs of the joints.
- Since the musculoskeletal system has a major impact on a person’s well-being and ability to function, begin by taking a detailed health history.
- The physical exam of the musculoskeletal system uses inspection, palpation, and percussion. The exam includes assessment of gait, posture, cerebellar function, limb measurement, joints, and muscles.
- Once you have completed your assessment, analyze your findings, identify actual and potential health problems, and write nursing diagnoses and a plan of care.


