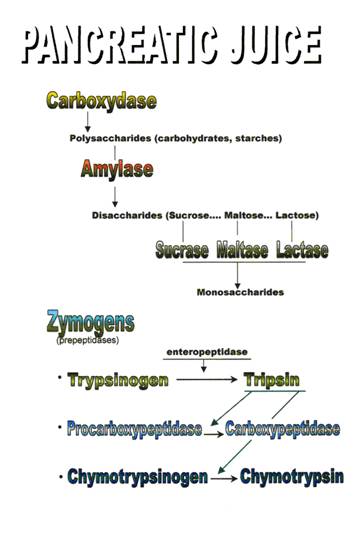
Digestion of proteins.
General and
specific pathways of amino acids transformation.
PROTEIN CATABOLISM –
hydrolysis breaks peptide bonds yielding amino acids
http://www.youtube.com/watch?v=SkkoE1RN_5E
AMINO ACID CATABOLISM -
(requires B6)
PROTEIN
CATABOLISM – attaches an amino group of an amino acid to a
keto acid converting a keto acid
into an amino acid. The original amino acid
becomes a keto acid.
1. New amino acid can be used for synthesis
2. Keto acid can be broken down in the TCA cycle
DEAMINATION – uses deaminase, water & NAD
1. breaks down an amino acid into a keto acid
and an ammonia.
2. liver cells convert ammonia to urea via the
PROTEIN ANABOLISM – dehydration synthesis
A. Amination – attaches amino group to a keto
acid
B. Ten essential amino acids
C. Deficiency diseases
1. marasmus
2. kwashiorkor
D. Genetic metabolic disorder - PKU
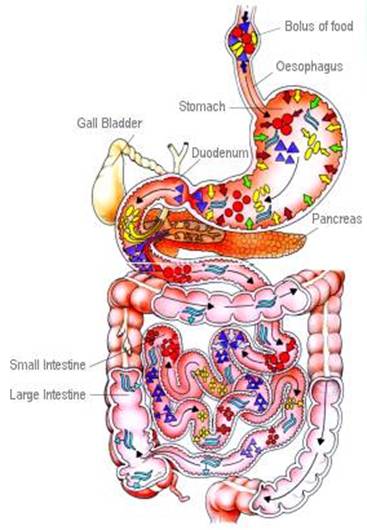
Breakdown of Food
and Fat
http://www.youtube.com/watch?v=AEsQxzeAry8
The
digestive process breaks down food by chemical and mechanical action into
substances that can pass into the bloodstream and be processed by body cells.
http://www.youtube.com/watch?v=g9G0zzdQx-M&feature=related
Certain
nutrients, such as salts and minerals, can be absorbed directly into the
circulation. Fat, complex carbohydrates, and proteins are broken down into
smaller molecules before being absorbed.
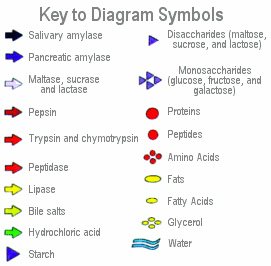
Fat
is split into glycerol and fatty acids; carbohydrates are split into
monosaccharide sugars; and proteins are split into linked amino acids called
peptides, and then into individual amino acids.
http://www.youtube.com/watch?v=STzOiRqzzL4
http://www.youtube.com/watch?v=tNdBdodTJNs&feature=related
http://www.youtube.com/watch?v=NewpaNwevFk
1: Mouth and oesophagus
Food
is chewed with the teeth and mixed with saliva. The enzyme amylase, present in
saliva, begins the breakdown of starch into sugar. Each lump of soft food,
called a bolus, is swallowed and propelled by contractions down the oesophagus
into the stomach.
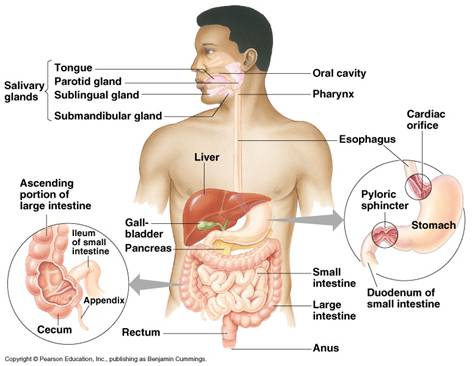
2: Stomach
Pepsin
is an enzyme produced when pepsinogen, a substance secreted by the stomach
lining, is modified by hydrochloric acid (also produced by the stomach lining).
http://www.youtube.com/watch?v=1jtYH3RihcA
Pepsin
breaks proteins down into smaller units, called polypeptides and peptides.
Lipase is a stomach enzyme that breaks down fat into glycerol and fatty acids.
The acid produced by the stomach also kills bacteria.
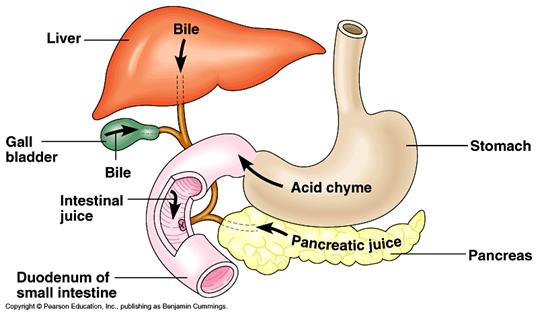
3: Duodenum
Lipase,
a pancreatic enzyme, breaks down fat into glycerol and fatty acids. Amylase,
another enzyme produced by the pancreas, breaks down starch into maltose, a
disaccharide sugar. Trypsin and chymotrypsin are powerful pancreatic enzymes
that split proteins into polypeptides and peptides.
4: Small Intestine
Maltase,
sucrase, and lactase are enzymes produced by the lining of the small intestine.
They convert disaccharide sugars into monosaccharide sugars. Peptidase, another
enzyme produced in the intestine, splits large peptides into smaller peptides
and then into amino acids.
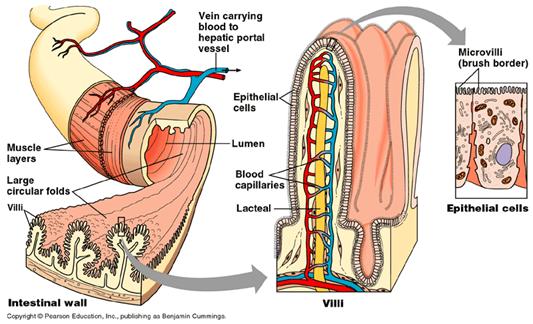
5: Large Intestine
Undigested food enters the large intestine, where
water and salt are absorbed by the intestinal lining. The residue, together
with waste pigments, dead cells , and bacteria, is pressed into faeces and
stored for excretion.
Urea Cycle
http://www.youtube.com/watch?v=AoBbVu5rnMs
Humans are
totally dependent on other organisms for converting atmospheric nitrogen into
forms available to the body. Nitrogen fixation is carried out by bacterial
nitrogensases forming reduced nitrogen, NH4+ which can
then be used by all organisms to form amino acids.
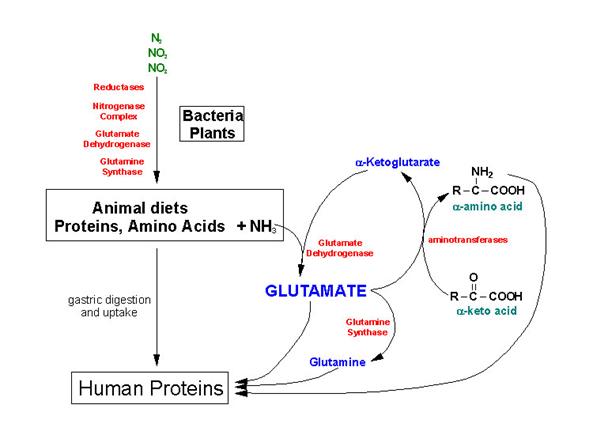
Overview of the flow of nitrogen in the biosphere.
Nitrogen, nitrites and nitrates are acted upon by bacteria (nitrogen fixation)
and plants and we assimilate these compounds as protein in our diets. Ammonia
incorporation in animals occurs through the actions of glutamate dehydrogenase
and glutamine synthase. Glutamate plays the central role in mammalian nitrogen
flow, serving as both a nitrogen donor and nitrogen acceptor.
Reduced nitrogen enters the human body as
dietary free amino acids, protein, and the ammonia produced by intestinal tract
bacteria. A pair of principal enzymes, glutamate dehydrogenase and glutamine
synthatase, are found in all organisms and effect the conversion of ammonia
into the amino acids glutamate and glutamine, respectively. Amino and amide groups
from these 2 substances are freely transferred to other carbon skeletons by transamination and transamidation
reactions.
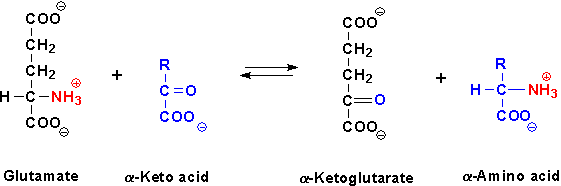
Representative aminotransferase catalyzed reaction.
Aminotransferases exist for all amino acids except threonine and lysine.
The most common compounds involved as a donor/acceptor pair in transamination
reactions are glutamate and -ketoglutarate (-KG), which participate in reactions with many
different aminotransferases. Serum aminotransferases such as serum
glutamate-oxaloacetate-aminotransferase (SGOT) (also called aspartate
aminotransferase, AST) and serum glutamate-pyruvate
aminotransferase (SGPT) (also called alanine transaminase, ALT)
have been used as clinical markers of tissue damage, with increasing serum
levels indicating an increased extent of damage. Alanine transaminase
has an important function in the delivery of skeletal muscle carbon and
nitrogen (in the form of alanine) to the liver. In skeletal muscle, pyruvate is
transaminated to alanine, thus affording an additional route of nitrogen
transport from muscle to liver. In the liver alanine transaminase
tranfers the ammonia to -KG and regenerates pyruvate. The pyruvate can then be
diverted into gluconeogenesis. This process is refered to as the glucose-alanine cycle.
The Glutamate Dehydrogenase Reaction
The reaction catalyzed by glutamate dehydrogenase is:
NH4++-ketoglutarate+NAD(P)H+H+<---->glutamate+NAD(P)++H2O
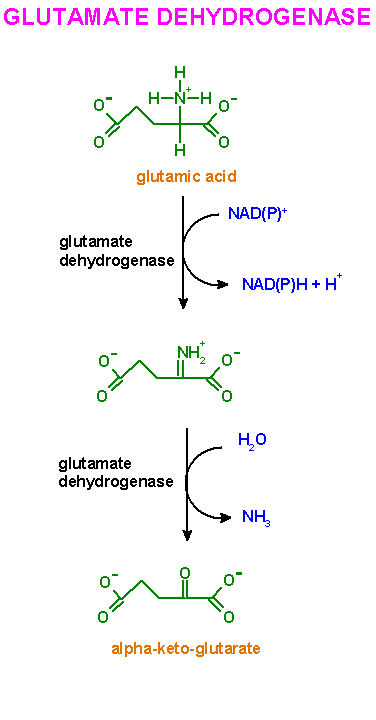
Glutamate dehydrogenase can utilize either NAD orNADP
as cofactor. In the forward reaction as shown above glutamate
dehydrogenase is important in converting free ammonia and -ketoglutarate (-KG) to glutamate, forming one
of the 20 amino acids required for protein synthesis. However, it should be
recognized that the reverse reaction is a key anapleurotic process linking
amino acid metabolism with TCA cycle activity.In the reverse reaction, glutamate
dehydrogenase provides an oxidizable carbon source used for the
production of energy as well as a reduced electron carrier, NADH. As expected
for a branch point enzyme with an important link to energy metabolism, glutamate
dehydrogenase is regulated by the cell energy charge. ATP and GTP are
positive allosteric effectors of the formation of glutamate, whereas ADP and
GDP are positive allosteric effectors of the reverse reaction. Thus, when the
level of ATP is high, conversion of glutamate to -KG and other TCA cycle
intermediates is limited; when the cellular energy charge is low, glutamate is
converted to ammonia and oxidizable TCA cycle intermediates. Glutamate is also
a principal amino donor to other amino acids in subsequent transamination
reactions. The multiple roles of glutamate in nitrogen balance make it a
gateway between free ammonia and the amino groups of most amino acids.
The Glutamine Synthase Reaction
The reaction
catalyzed by glutamine synthase is:
glutamate +
NH4+ + ATP -------> glutamine + ADP + Pi +
H+
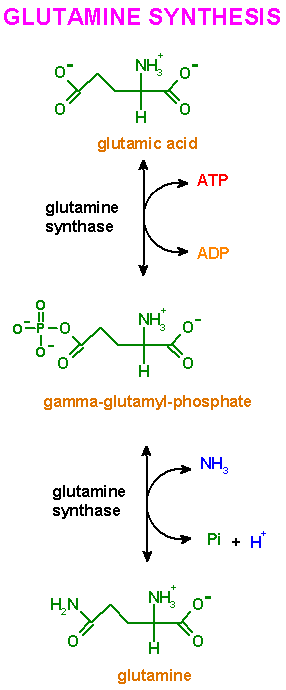
The glutamine
synthatase reaction is also important in several respects. First it
produces glutamine, one of the 20 major amino acids. Second, in animals,
glutamine is the major amino acid found in the circulatory system. Its role
there is to carry ammonia to and from various tissues but principally from
peripheral tissues to the kidney, where the amide nitrogen is hydrolyzed by the
enzyme glutaminase (reaction below); this process regenerates
glutamate and free ammonium ion, which is excreted in the urine.
glutamine + H2O -------> glutamate + NH3
Note that, in this function, ammonia arising in
peripheral tissue is carried in a nonionizable form which has none of the
neurotoxic or alkalosis-generating properties of free ammonia.
Liver
contains both glutamine synthetase and glutaminase
but the enzymes are localized in different cellular segments. This ensures that
the liver is neither a net producer nor consumer of glutamine. The differences
in cellular location of these two enzymes allows the liver to scavange ammonia
that has not been incorporated into urea. The enzymes of the urea cycle are
located in the same cells as those that contain glutaminase. The
result of the differential distribution of these two hepatic enzymes makes it
possible to control ammonia incorporation into either urea or glutamine, the
latter leads to excretion of ammonia by the kidney.
When acidosis occurs the body will divert more glutamine from the liver to the
kidney. This allows for the conservation of bicarbonate ion since the
incorporation of ammonia into urea requires bicarbonate (see below). When
glutamine enters the kidney, glutaminase releases one mole of
ammonia generating glutamate and then glutamate dehydrogenase
releases another mole of ammonia generating a-ketoglutarate. The ammonia will
ionizes to ammonium ion ( NH4+) which is excreted. The
net effect is a reduction in the pH (see also Kidneys and Acid-Base Balance).
While glutamine, glutamate, and the remaining nonessential amino acids can
be made by animals, the majority of the amino acids found in human tissues necessarily
come from dietary sources (about 400g of protein per day). Protein digestion
begins in the stomach, where a proenzyme called pepsinogen is
secreted, autocatalytically converted to Pepsin A, and used for
the first step of proteolysis. However, most proteolysis takes place in the
duodenum as a consequence of enzyme activities secreted by the pancreas. All of
the serine proteases and the zinc peptidases of pancreatic secretions are
produced in the form of their respective proenzymes. These proteases are both
endopeptidase and exopeptidase, and their combined action in the intestine
leads to the production of amino acids, dipeptides, and tripeptides, all of
which are taken up by enterocytes of the mucosal wall.
A circuitous regulatory pathway leading to the secretion of proenzymes into the
intestine is triggered by the appearance of food in the intestinal lumen.
Special mucosal endocrine cells secret the peptide hormones cholecystokinin (CCK) and secretin
into the circulatory system. Together, CCK and secretin cause contraction of
the gall bladder and the exocrine secretion of a bicarbonate-rich, alkaline
fluid, containing protease proenzymes from the pancreas into the intestine. A
second, paracrine role of CCK is to stimulate adjacent intestinal cells to
secrete enteropeptidase, a protease that cleaves trypsinogen
to produce trypsin. Trypsin also activates trypsinogen
as well as all the other proenzymes in the pancreatic secretion, producing the
active proteases and peptidases that hydrolyze dietary polypeptides.
Subsequent to luminal hydrolysis, small peptides and amino acids are
transferred through enterocytes to the portal circulation by diffusion,
facilitated diffusion, or active transport. A number of Na+-dependent
amino acid transport systems with overlapping amino acid specificity have been
described. In these transport systems, Na+ and amino acids at high
luminal concentrations are co-transported down their concentration gradient to
the interior of the cell. The ATP-dependent Na+/K+ pump
exchanges the accumulated Na+ for extracellular K+,
reducing intracellular Na+ levels and maintaining the high
extracellular Na+ concentration (high in the intestinal lumen, low
in enterocytes) required to drive this transport process.
Transport mechanisms of this nature are ubiquitous in the body. Small peptides
are accumulated by a proton (H+) driven transport process and
hydrolyzed by intracellular peptidases. Amino acids in the circulatory system
and in extracellular fluids are transported into cells of the body by at least
7 different ATP-requiring active transport systems with overlapping amino acid
specificities.
Hartnup disorder is an autosomal recessive impairment of neutral amino
acid transport affecting the kidney tubules and small intestine. It is believed
that the defect lies in a specific system responsible for neutral amino acid
transport across the brush-border membrane of renal and intestinal epithelium.
The exact defect has not yet been characterized. The characteristic diagnostic
feature of Hartnup disorder is a dramatic neutral hyperaminoaciduria.
Additionally, individuals excrete indolic compounds that originate from the
bacterial degradation of unabsorbed tryptophan. The reduced intestinal
absorption and increased renal loss of tryptophan lead to a reduced
availability of tryptophan for niacin and nicotinamide nucleotide biosynthesis.
As a consequence affected individuals frequently exhibit pellegra-like rashes.
.
Many other
nitrogenous compounds are found in the intestine. Most are bacterial products
of protein degradation. Some have powerful pharmacological (vasopressor)
effects.
|
Products of Intestinal Bacterial Activity |
||
|
Substrates |
Products |
|
|
- |
Vasopressor Amines |
Other |
|
Lysine |
Cadaverene |
- |
|
Arginine |
Agmatine |
- |
|
Tyrosine |
Tyramine |
- |
|
Ornithine |
Putrescine |
- |
|
Histidine |
Histamine |
- |
|
Tryptophan |
- |
Indole and
skatole |
|
All amino
acids |
- |
NH4+ |
Prokaryotes
such as E. coli can make the carbon skeletons of all 20 amino acids and
transaminate those carbon skeletons with nitrogen from glutamine or glutamate
to complete the amino acid structures. Humans cannot synthesize the branched
carbon chains found in branched chain amino acids or the ring systems found in
phenylalanine and the aromatic amino acids; nor can we incorporate sulfur into
covalently bonded structures. Therefore, the 10 so-called essential amino acids must be supplied from the diet.
Nevertheless, it should be recognized that,depending on the composition of the
diet and physiological state of an individual,one or another of the
non-essential amino acids may also become a required dietary component. For
example, arginine is not usually considered to be essential, because enough for
adult needs is made by the urea cycle.
However, the
urea cycle generally does not provide sufficient arginine for the needs of a
growing child.
To take a different type of example, cysteine and
tyrosine are considered non-essential but are formed from the essential amino
acids methionine and phenylalanine, respectively. If sufficient cysteine and
tyrosine are present in the diet, the requirements for methionine and
phenylalanine are markedly reduced; conversely, if methionine and phenylalanine
are present in only limited quantities, cysteine and tyrosine can become
essential dietary components. Finally, it should be recognized that if the -keto acids corresponding to the carbon skeleton of
the essential amino acids are supplied in the diet, aminotransferases in the
body will convert the keto acids to their respective amino acids, largely
supplying the basic needs.
Unlike fats and carbohydrates, nitrogen has no designated storage depots in the
body. Since the half-life of many proteins is short (on the order of hours),
insufficient dietary quantities of even one amino acid can quickly limit the
synthesis and lower the body levels of many essential proteins. The result of
limited synthesis and normal rates of protein degradation is that the balance
of nitrogen intake and nitrogen excretion is rapidly and significantly altered.
Normal, healthy adults are generally in nitrogen
balance, with intake and excretion being very well matched. Young
growing children, adults recovering from major illness, and pregnant women are
often in positive nitrogen balance. Their intake
of nitrogen exceeds their loss as net protein synthesis proceeds. When more
nitrogen is excreted than is incorporated into the body, an individual is in negative nitrogen balance. Insufficient quantities of
even one essential amino acid is adequate to turn an otherwise normal
individual into one with a negative nitrogen balance. The biological value of
dietary proteins is related to the extent to which they provide all the
necessary amino acids. Proteins of animal origin generally have a high
biological value; plant proteins have a wide range of values from almost none
to quite high. In general, plant proteins are deficient in lysine, methionine,
and tryptophan and are much less concentrated and less digestible than animal
proteins. The absence of lysine in low-grade cereal proteins, used as a dietary
mainstay in many underdeveloped countries, leads to an inability to synthesize
protein (because of missing essential amino acids) and ultimately to a syndrome
known as kwashiorkor, common among children in
these countries.
Essential vs. Nonessential Amino Acids
|
Nonessential |
Essential |
|
Alanine |
Arginine* |
|
Asparagine |
Histidine |
|
Aspartate |
Isoleucine |
|
Cysteine |
Leucine |
|
Glutamate |
Lysine |
|
Glutamine |
Methionine* |
|
Glycine |
Phenylalanine* |
|
Proline |
Threonine |
|
Serine |
Tryptophan |
|
Tyrosine |
Valine |
|
The amino acids arginine,
methionine and phenylalanine
are considered essential for reasons not directly related to lack of
synthesis. Arginine is synthesized by mammalian cells but at a rate that is
insufficient to meet the growth needs of the body and the majority that is
synthesized is cleaved to form urea. Methionine is required in large amounts
to produce cysteine if the latter amino acid is not adequately supplied in
the diet. Similarly, phenyalanine is needed in large amounts to form tyrosine
if the latter is not adequately supplied in the diet. |
|
Removal of Nitrogen
from Amino Acids
http://www.youtube.com/watch?v=5pBNunRmJn4
Nitrogen elimination begins intracellularly with
protein degradation. There are two main routes for converting intracellular
proteins to free amino acids: a lysosomal pathway, by which extracellular and
some intracellular proteins are degraded, and cytosolic pathways that are
important in degrading proteins of intracellular origin. In one cytosolic
pathway a protein known as ubiquitin is activated by conversion to an AMP derivative, and
cytosolic proteins that are damaged or otherwise destined for degradation are
enzymically tagged with the activated ubiquitin. Ubiquitin-tagged proteins are
then attacked by cytosolic ATP-dependent proteases that hydrolyze the targeted
protein, releasing the ubiquitin for further rounds of protein targeting.
The dominant reactions involved in removing amino acid nitrogen from the
body are known as transaminations. This class of
reactions funnels nitrogen from all free amino acids into a small number of
compounds; then, either they are oxidatively deaminated, producing ammonia, or
their amine groups are converted to urea by the urea cycle. Transaminations
involve moving an -amino group from a donor a-amino acid to the keto
carbon of an acceptor -keto acid. These reversible reactions are catalyzed
by a group of intracellular enzymes known as aminotransferases
(transaminases), which employ covalently bound pyridoxal phosphate as a
cofactor (see reaction mechanism).
Aminotransferases exist for all amino acids except
threonine and lysine. The most common compounds involved as a donor/acceptor
pair in transamination reactions are glutamic acid and -ketoglutaric acid, which participate in reactions
with many different aminotransferases. Serum aminotransferases such as serum
glutamate - oxaloacetate
- aminotransferase (SGOT) have been used as clinical markers of tissue
damage, with increasing serum levels indicating an increased extent of damage.
A small but clinically
important amount of creatinine is excreted in the urine daily, and the creatinine
clearance rate is often used as an indicator of kidney function. The
first reaction in creatinine formation is the transfer of the amido (or
amidine) group of arginine to glycine, forming guanidinoacetate. Subsequently,
a methyl group is transferred from the ubiquitous 1-carbon-donor S-adenosylmethionine
to guanidinoacetate to produce creatine (from which phosphocreatine is formed),
some of which spontaneously cyclizes to creatinine, and is eliminated in the
urine. The quantity of urine creatinine is generally constant for an individual
and approximately proportional to muscle mass. In individuals with damaged
muscle cells, creatine leaks out of the damaged tissue and is rapidly cyclized,
greatly increasing the quantity of circulating and urinary creatinine.
Because of the participation of -ketoglutarate in numerous transaminations,
glutamate is a prominent intermediate in nitrogen elimination as well as in
anabolic pathways. Glutamate formed in the course of nitrogen elimination is
either oxidatively deaminated by liver glutamate dehydrogenase,
forming ammonia, or converted to glutamine by glutamine synthase
and transported to kidney tubule cells. There the glutamine is sequentially
deamidated by glutaminase and deaminated by kidney glutamate
dehydrogenase.
The ammonia produced in the latter two reactions
is excreted as NH4+ in the urine, where it helps maintain
urine pH in the normal range of pH 4 to pH 8. The extensive production of
ammonia by peripheral or liver glutamate dehydrogenase is not
feasible because of the highly toxic effects of circulating ammonia. Normal
serum ammonium concentrations are in the range of 20-40 mmol, and an increase
in circulating ammonia to about 400 mmol causes alkalosis and neurotoxicity.
A final, therapeutically useful amino acid-related reaction is the amidation of
aspartic acid to produce asparagine. The enzyme asparagine synthase
catalyzes the ATP, requiring the transamidation reaction shown below:
aspartate+glutamine+ATP-------->glutamate+asparagine+AMP+PPi
Most cells perform this reaction well enough to produce all the asparagine
they need. However, some leukemia cells require exogenous asparagine, which
they obtain from the plasma. Chemotherapy using the enzyme asparaginase
takes advantage of this property of leukemic cells by hydrolyzing serum
asparagine to ammonia and aspartic acid, thus depriving the neoplastic cells of
the asparagine that is essential for their characteristic rapid growth.
In the peroxisomes of mammalian tissues, especially liver, there are 2 stereospecific
amino acid oxidases involved in elimination of amino acid
nitrogen. D-amino acid oxidase is an FAD-linked enzyme, and while
there are few D-amino acids that enter the human body the activity of this
enzyme in liver is quite high. L-amino acid oxidase is FMN-linked
and has broad specificity for the L amino acids.A number of substances,
including oxygen, can act as electron acceptors from the flavoproteins. If
oxygen is the acceptor the product is hydrogen peroxide, which is then rapidly
degraded by the catalases found in liver and other tissues. Missing or defective biogenesis of peroxisomes or L-amino acid
oxidase causes generalized hyper-aminoacidemia and hyper-aminoaciduria,
generally leading to neurotoxicity and early death.
Amino Acid Biosynthesis
http://www.youtube.com/watch?v=VXZuuo3DD4s
Glutamate
and Aspartate
Glutamate and aspartate are synthesized from their
widely distributed -keto acid precursors by simple 1-step transamination reactions. The former
catalyzed by glutamate dehydrogenase and the latter by aspartate
aminotransferase, AST.Aspartate is also derived from asparagine
through the action of asparaginase. The importance of glutamate as a
common intracellular amino donor for transamination reactions and of aspartate
as a precursor of ornithine for the urea cycle is described in the Nitrogen Metabolism page.
Alanine and the Glucose-Alanine Cycle
Aside
from its role in protein synthesis, alanine is second only to glutamine in
prominence as a circulating amino acid. In this capacity it serves a unique
role in the transfer of nitrogen from peripheral tissue to the liver. Alanine
is transferred to the circulation by many tissues, but mainly by muscle, in
which alanine is formed from pyruvate at a rate proportional to intracellular
pyruvate levels. Liver accumulates plasma alanine, reverses the transamination
that occurs in muscle, and proportionately increases urea production. The
pyruvate is either oxidized or converted to glucose via gluconeogenesis. When alanine transfer from muscle to liver is
coupled with glucose transport from liver back to muscle, the process is known
as the glucose-alanine cycle. The key feature of the cycle is that in 1
molecule, alanine, peripheral tissue exports pyruvate and ammonia (which are
potentially rate-limiting for metabolism) to the liver, where the carbon
skeleton is recycled and most nitrogen eliminated.There are 2 main pathways to
production of muscle alanine: directly from protein degradation, and via the
transamination of pyruvate by glutamate-pyruvate aminotransferase
(also called alanine transaminase, ALT).
glutamate + pyruvate <-------> -KG + alanine
The sulfur for cysteine synthesis comes from the
essential amino acid methionine. A condensation of ATP and methionine catalyzed
by methionine adenosyltransferase yields S-adenosylmethionine (SAM or AdoMet).
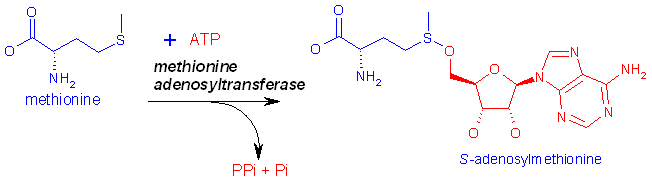
Biosynthesis of S-adenosylmethionine, SAM
SAM
serves as a precurosor for numerous methyl transfer reactions (e.g. the
conversion of norepinephrine to epinenephrine, see Specialized Products of Amino Acids). The result of methyl transfer is the
conversion of SAM to S-adenosylhomocysteine. S-adenosylhomocysteine is then
cleaved by adenosylhomocyteinase to yield homocysteine and adenosine.
Homocysteine can be converted back to methionine by methionine synthase,
a reaction that occurs under methionine-sparing conditions and requires N5-methyl-tetrahydrofolate
as methyl donor. This reaction was discussed in the context of vitamin B12-requiring
enzymes in the Vitamins page. Transmethylation reactions employing SAM are
extremely important, but in this case the role of S-adenosylmethionine in
transmethylation is secondary to the production of homocysteine (essentially a
by-product of transmethylase activity). In the production of SAM all
phosphates of an ATP are lost: one as Pi and two as PPi.
It is adenosine which is transferred to methionine and not AMP. In cysteine
synthesis, homocysteine condenses with serine to produce cystathionine, which
is subsequently cleaved by cystathionase to produce cysteine and -ketobutyrate. The sum of the latter two
reactions is known as trans-sulfuration. Cysteine is used for protein
synthesis and other body needs, while the ketobutyrate is decarboxylated and converted to
propionyl-CoA. While cysteine readily oxidizes in air to form the disulfide
cystine, cells contain little if any free cystine because the ubiquitous
reducing agent, glutathione effectively reverses the formation of
cystine by a non-enzymatic reduction reaction.
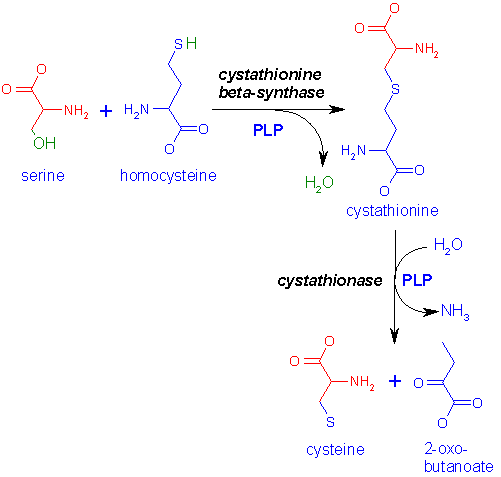
Utilization of methionine in the synthesis of
cysteine
The
2 key enzymes of this pathway, cystathionine synthase and cystathionase
(cystathionine lyase), both use pyridoxal phosphate as a cofactor, and both
are under regulatory control. Cystathionase is under negative allosteric
control by cysteine, as well, cysteine inhibits the expression of the cystathionine
synthase gene. Genetic defects are known for both the synthase and the
lyase. Missing or impaired cystathionine synthase leads to homocystinuria and is often associated with mental retardation,
although the complete syndrome is multifaceted and many individuals with this
disease are mentally normal. Some instances of genetic homocystinuria respond
favorably to pyridoxine therapy, suggesting that in these cases the defect in cystathionine
synthase is a decreased affinity for the cofactor. Missing or impaired cystathionase
leads to excretion of cystathionine in the urine but does not have any other
untoward effects. Rare cases are known in which cystathionase is
defective and operates at a low level. This genetic disease leads to
methioninuria with no other consequences.
Tyrosine Biosynthesis
Tyrosine
is produced in cells by hydroxylating the essential amino acid phenylalanine.
This relationship is much like that between cysteine and methionine. Half of
the phenylalanine required goes into the production of tyrosine; if the diet is
rich in tyrosine itself, the requirements for phenylalanine are reduced by
about 50%. Phenylalanine hydroxylase is a mixed-function
oxygenase: one atom of oxygen is incorporated into water and the other into the
hydroxyl of tyrosine. The reductant is the tetrahydrofolate-related cofactor tetrahydrobiopterin, which is maintained in the reduced state by the
NADH-dependent enzyme dihydropteridine reductase.
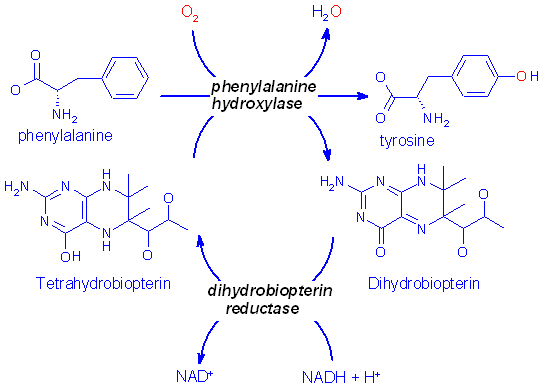
Biosynthesis of tyrosine from phenylalanine
Missing
or deficient phenylalanine hydroxylase leads to the genetic
disease known as phenlyketonuria (PKU), which if untreated leads to severe mental
retardation. The mental retardation is caused by the accumulation of
phenylalanine, which becomes a major donor of amino groups in aminotransferase
activity and depletes neural tissue of -ketoglutarate. This absence of -ketoglutarate in the brain shuts down the TCA cycle and the associated production of aerobic energy,
which is essential to normal brain development.
The
product of phenylalanine transamination, phenylpyruvic acid, is reduced to
phenylacetate and phenyllactate, and all 3 compounds appear in the urine. The
presence of phenylacetate in the urine imparts a "mousy" odor. If the
problem is diagnosed early, the addition of tyrosine and restriction of
phenylalanine from the diet can minimize the extent of mental retardation.
In
other pathways, tetrahydrobiopterin is a cofactor. The effects of missing or
defective dihydropteridine reductase cause even more severe
neurological difficulties than those usually associated with PKU caused by
deficient hydroxylase activity.
Ornithine and Proline Biosynthesis
Glutamate
is the precursor of both proline and ornithine, with glutamate semialdehyde
being a branch point intermediate leading to one or the other of these 2
products. While ornithine is not one of the 20 amino acids used in protein
synthesis, it plays a significant role as the acceptor of carbamoyl phosphate
in the urea cycle. Ornithine serves an additional important role as the
precursor for the synthesis of the polyamines. The production of ornithine from glutamate is
important when dietary arginine, the other principal source of ornithine, is
limited. The fate of glutamate semialdehyde depends on prevailing cellular
conditions. Ornithine production occurs from the semialdehyde via a simple
glutamate-dependent transamination, producing ornithine.
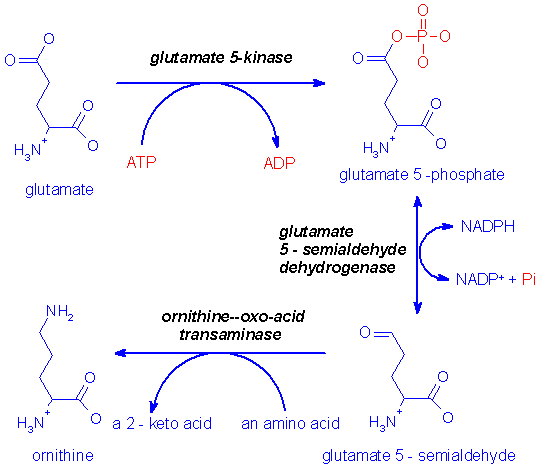
Ornithine synthesis from glutamate
When
arginine concentrations become elevated, the ornithine contributed from the urea cycle plus that from glutamate semialdehyde inhibit
the aminotransferase reaction, with accumulation of the semialdehyde as a
result. The semialdehyde cyclizes spontaneously to 1pyrroline-5-carboxylate which is then reduced to proline by an
NADPH-dependent reductase.
The
main pathway to serine starts with the glycolytic intermediate
3-phosphoglycerate.
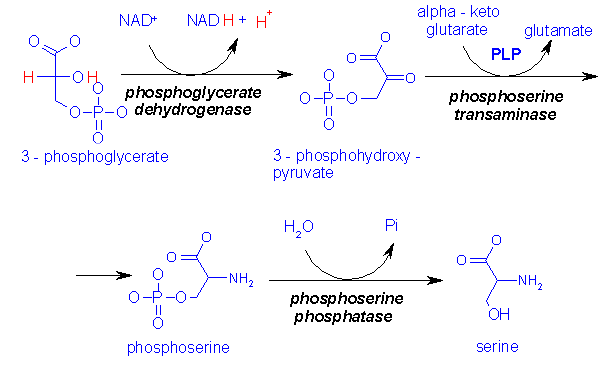
An
NADH-linked dehydrogenase converts 3-phosphoglycerate into a keto acid,
3-phosphopyruvate, suitable for subsequent transamination. Aminotransferase
activity with glutamate as a donor produces 3-phosphoserine, which is converted
to serine by phosphoserine phosphatase.
The
main pathway to glycine is a 1-step reaction catalyzed by serine
hydroxymethyltransferase.
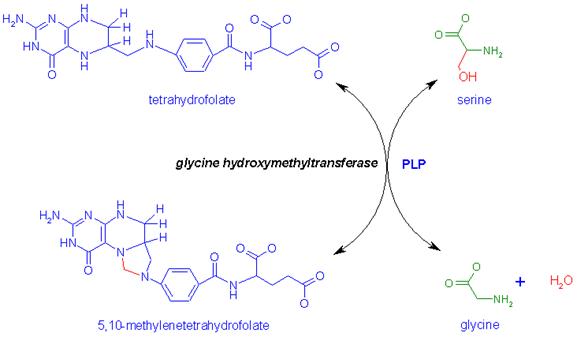
This
reaction involves the transfer of the hydroxymethyl group from serine to the
cofactor tetrahydrofolate (THF), producing glycine and N5,N10-methylene-THF.
Glycine produced from serine or from the diet can also be oxidized by glycine
cleavage complex, GCC, to yield a second equivalent of N5,N10-methylene-tetrahydrofolate
as well as ammonia and CO2.
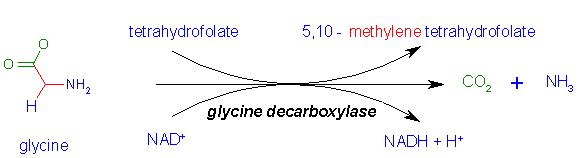
Glycine
is involved in many anabolic reactions other than protein synthesis including
the synthesis of purine nucleotides, heme, glutathione, creatine and serine.
Aspartate/Asparagine
and Glutamate/Glutamine Biosynthesis
Glutamate
is synthesized by the reductive amination of -ketoglutarate catalyzed by glutamate
dehydrogenase; it is thus a nitrogen-fixing reaction. In addition,
glutamate arises by aminotransferase reactions, with the amino nitrogen being
donated by a number of different amino acids. Thus, glutamate is a general
collector of amino nitrogen. Aspartate is formed in a transamintion reaction
catalyzed by aspartate transaminase, AST. This reaction uses the
aspartate -keto acid analog, oxaloacetate, and glutamate
as the amino donor. Aspartate can also be formed by deamination of asparagine
catalyzed by asparaginase. Asparagine synthetase
and glutamine synthetase, catalyze the production of asparagine
and glutamine from their respective amino acids. Glutamine is produced from
glutamate by the direct incorporation of ammonia; and this can be considered
another nitrogen fixing reaction. Asparagine, however, is formed by an
amidotransferase reaction. Aminotransferase reactions are readily reversible.
The direction of any individual transamination depends principally on the
concentration ratio of reactants and products. By contrast, transamidation
reactions, which are dependent on ATP, are considered irreversible. As a
consequence, the degradation of asparagine and glutamine take place by a
hydrolytic pathway rather than by a reversal of the pathway by which they were
formed. As indicated above, asparagine can be degraded to aspartate.
Amino Acid Catabolism
Glutamine/Glutamate and Asparagine/Aspartate
Catabolism
Glutaminase is an important kidney tubule enzyme involved in
converting glutamine (from liver and from other tissue) to glutamate and NH3+,
with the NH3+ being excreted in the urine. Glutaminase
activity is present in many other tissues as well, although its activity is not
nearly as prominent as in the kidney. The glutamate produced from glutamine is
converted to -ketoglutarate, making glutamine a glucogenic
amino acid. Asparaginase is also widely distributed within the
body, where it converts asparagine into ammonia and aspartate. Aspartate
transaminates to oxaloacetate, which follows the gluconeogenic pathway to
glucose. Glutamate and aspartate are important in collecting and eliminating
amino nitrogen via glutamine synthetase and the urea cycle, respectively. The catabolic path of the carbon
skeletons involves simple 1-step aminotransferase reactions that directly
produce net quantities of a TCA cycle intermediate. The glutamate dehydrogenase
reaction operating in the direction of -ketoglutarate production provides a second
avenue leading from glutamate to gluconeogenesis.
Alanine is also important in intertissue nitrogen
transport as part of the glucose-alanine cycle. Alanine's catabolic pathway involves a simple
aminotransferase reaction that directly produces pyruvate. Generally pyruvate
produced by this pathway will result in the formation of oxaloacetate, although
when the energy charge of a cell is low the pyruvate will be oxidized to CO2
and H2O via the PDH complex and the TCA cycle. This makes alanine a glucogenic amino acid.
Arginine,
Ornithine and Proline Catabolism
The catabolism of arginine begins within the context
of the urea cycle. It is hydrolyzed to urea and ornithine by arginase.
Ornithine, in excess of urea cycle needs, is transaminated to form glutamate
semialdehyde. Glutamate semialdehyde can serve as the precursor for proline
biosynthesis as described above or it can be converted to glutamate. Proline
catabolism is a reversal of its synthesis process. The glutamate semialdehyde
generated from ornithine and proline catabolism is oxidized to glutamate by an
ATP-independent glutamate semialdehyde dehydrogenase. The
glutamate can then be converted to ketoglutarate in a transamination reaction. Thus
arginine, ornithine and proline, are glucogenic.
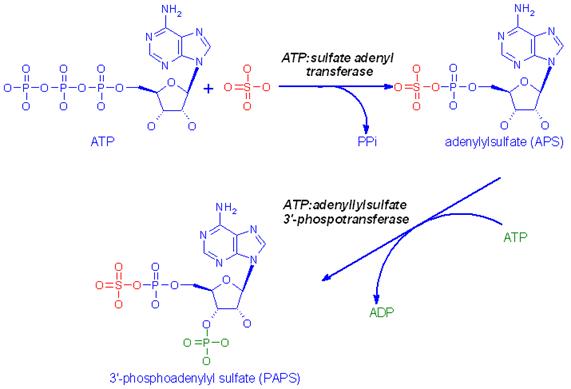
PAPS is used for the transfer of sulfate to biological
molecules such as the sugars of the glycosphingolipids.Other than protein, the most important product
of cysteine metabolism is the bile salt precursor taurine, which is used to form the bile acid conjugates taurocholate and taurochenodeoxycholate.The enzyme cystathionase can also
transfer the sulfur from one cysteine to another generating thiocysteine and
pyruvate. Transamination of cysteine yields -mercaptopyruvate which then reacts with
sulfite, (SO32-), to produce thiosulfate, (S2O32-)
and pyruvate. Both thiocysteine and thiosulfate can be used by the enzyme rhodanese
to incorporate sulfur into cyanide, (CN-), thereby detoxifying the
cyanide to thiocyanate.
The principal fates of the essential amino acid
methionine are incorporation into polypeptide chains, and use in the production
of -ketobutyrate and cysteine via SAM as described
above. The transulfuration reactions that produce cysteine from homocysteine
and serine also produce -ketobutyrate, the latter being converted to succinyl-CoA. Regulation of
the methionine metabolic pathway is based on the availability of methionine and
cysteine. If both amino acids are present in adequate quantities, SAM accumulates
and is a positive effector on cystathionine synthase, encouraging
the production of cysteine and ketobutyrate (both of which are glucogenic).
However, if methionine is scarce, SAM will form only in small quantities, thus
limiting cystathionine synthase activity. Under these conditions
accumulated homocysteine is remethylated to methionine, using N5-methylTHF
and other compounds as methyl donors.
Valine, Leucine
and Isoleucine Catabolism
This group of essential amino acids are identified as
the branched-chain amino
acids, BCAAs. Because
this arrangement of carbon atoms cannot be made by humans, these amino acids
are an essential element in the diet. The catabolism of all three compounds
initiates in muscle and yields NADH and FADH2 which can be utilized
for ATP generation. The catabolism of all three of these amino acids uses the
same enzymes in the first two steps. The first step in each case is a
transamination using a single BCAA aminotransferase, with -ketoglutarate as amine acceptor. As a result,
three different -keto acids are produced and are oxidized using a common branched-chain
-keto acid dehydrogenase, yielding the three different CoA derivatives.
Subsequently the metabolic pathways diverge, producing many intermediates. The
principal product from valine is propionylCoA, the glucogenic precursor of
succinyl-CoA. Isoleucine catabolism terminates with production of acetylCoA and
propionylCoA; thus isoleucine is both glucogenic and ketogenic. Leucine gives
rise to acetylCoA and acetoacetylCoA, and is thus classified as strictly
ketogenic. There are a number of genetic diseases associated with faulty
catabolism of the BCAAs. The most common defect is in the branched-chain -keto acid dehydrogenase. Since there is only one dehydrogenase enzyme
for all three amino acids, all three keto acids accumulate and are excreted in the
urine. The disease is known as Maple syrup urine disease because of the characteristic odor of the urine
in afflicted individuals. Mental retardation in these cases is extensive.
Unfortunately, since these are essential amino acids, they cannot be heavily
restricted in the diet; ultimately, the life of afflicted individuals is short
and development is abnormal The main neurological problems are due to poor
formation of myelin in the CNS.
Phenylalanine
and Tyrosine Catabolism
Phenylalanine normally has only two fates:
incorporation into polypeptide chains, and production of tyrosine via the
tetrahydrobiopterin-requiring phenylalanine hydroxylase. Thus,
phenylalanine catabolism always follows the pathway of tyrosine catabolism. The
main pathway for tyrosine degradation involves conversion to fumarate and
acetoacetate, allowing phenylalanine and tyrosine to be classified as both
glucogenic and ketogenic. Tyrosine is equally important for protein
biosynthesis as well as an intermediate in the biosynthesis of several
physiologically important metabolites e.g. dopamine, norepinephrine and
epinephrine (see Specialized Products of Amino Acids). As in phenylketonuria (deficiency of phenylalanine
hydroxylase), deficiency of tyrosine transaminase leads
to urinary excretion of tyrosine and the intermediates between phenylalanine
and tyrosine. The adverse neurological symptoms are the same for the two
diseases. Genetic diseases (such as various tyrosinemias and alkaptonuria) are
also associated with other defective enzymes of the tyrosine catabolic pathway.
The first genetic disease ever recognized, alcaptonuria, is caused by defective homogentisic acid
oxidase. Homogentisic acid accumulation is relatively innocuous,
causing urine to darken on exposure to air, but no life-threatening effects
accompany the disease. The other genetic deficiencies lead to more severe
symptoms, most of which are associated with abnormal neural development, mental
retardation, and shortened life span.
Lysine catabolism is unusual in the way that the -amino group is transferred to -ketoglutarate and into the general nitrogen
pool. The reaction is a transamination in which the -amino group is transferred to the -keto carbon of -ketoglutarate forming the metabolite, saccharopine. Unlike the majority of transamination reactions,
this one does not employ pyridoxal phosphate as a cofactor. Saccharopine is
immediately hydrolyzed by the enzyme -aminoadipic semialdehyde synthase in such a way that the amino nitrogen remains
with the -carbon of -ketoglutarate, producing glutamate and -aminoadipic semialdehyde. Because this
transamination reaction is not reversible, lysine is an essential amino acid.
The ultimate end-product of lysine catabolism is acetoacetyl-CoA Genetic
deficiencies in the enzyme -aminoadipic semialdehyde synthase have been observed in individuals who excrete
large quantities of urinary lysine and some saccharopine. The lysinemia and
associated lysinuria are benign. Other serious disorders associated with lysine
metabolism are due to failure of the transport system for lysine and the other
dibasic amino acids across the intestinal wall. Lysine is essential for protein
synthesis; a deficiencies of its transport into the body can cause seriously
diminished levels of protein synthesis. Probably more significant however, is
the fact that arginine is transported on the same dibasic amino acid carrier,
and resulting arginine deficiencies limit the quantity of ornithine available
for the urea cycle. The result is severe hyperammonemia after a meal
rich in protein. The addition of citrulline to the diet prevents the
hyperammonemia. Lysine is also important as a precursor for the synthesis of carnitine, required for the transport of fatty acids into the
mitochondria for oxidation. Free lysine does not serve as the precursor for
this reaction, rather the modified lysine found in certain proteins. Some
proteins modify lysine to trimethyllysine using SAM as the methyl donor to transfer
methyl groups to the -amino of the lysine side chain. Hydrolysis of proteins containing
trimethyllysine provide the substrate for the subsequent conversion to
carnitine.
Histidine catabolism begins with release of the amino group catalyzed by histidase,
introducing a double bond into the molecule. As a result, the deaminated
product, urocanate, is not the usual -keto acid associated with loss of -amino nitrogens. The end product of histidine
catabolism is glutamate, making histidine one of the glucogenic amino acids.
Another key feature of histidine catabolism is that it serves as a source of
ring nitrogen to combine with tetrahydrofolate (THF), producing the 1-carbon
THF intermediate known as N5-formiminoTHF. The latter
reaction is one of two routes to N5-formiminoTHF. The
principal genetic deficiency associated with histidine metabolism is absence or
deficiency of the first enzyme of the pathway, histidase. The
resultant histidinemia is relatively benign. The disease, which is of
relatively high incidence (
Tryptophan Catabolism
A number of important side reactions occur during the
catabolism of tryptophan on the pathway to acetoacetate. The first enzyme of
the catabolic pathway is an iron porphyrin oxygenase that opens the indole
ring. The latter enzyme is highly inducible, its concentration rising almost
10-fold on a diet high in tryptophan. Kynurenine is the first key
branch point intermediate in the pathway. Kynurenine undergoes deamniation in a
standard transamination reaction yielding kynurenic acid. Kynurenic acid
and metabolites have been shown to act as antiexcitotoxics and anticonvulsives.
A second side branch reaction produces anthranilic acid plus alanine. Another equivalent of alanine is produced
further along the main catabolic pathway, and it is the production of these
alanine residues that allows tryptophan to be classified among the glucogenic
and ketogenic amino acids. The second important branch point converts
kynurenine into 2-amino-3-carboxymuconic semialdehyde, which has two fates. The
main flow of carbon elements from this intermediate is to glutarate. An
important side reaction in liver is a transamination and several rearrangements
to produce limited amounts of nicotinic
acid, which leads to
production of a small amount of NAD+ and NADP+ Aside form
its role as an amino acid in protein biosynthesis, tryptophan also serves as a
precursor for the synthesis of serotonin and melatonin. These products are discussed in Specialized Products of Amino Acids